Preoperative Radiological Parameters to Predict Clinical and Radiological Outcomes after Laminoplasty
Article information
Abstract
Many studies have focused on pre-operative sagittal alignment parameters which could predict poor clinical or radiological outcomes after laminoplasty. However, the influx of too many new factors causes confusion. This study reviewed sagittal alignment parameters, predictive of clinical or radiological outcomes, in the literature. Preoperative kyphotic alignment was initially proposed as a predictor of clinical outcomes. The clinical significance of the K-line and K-line variants also has been studied. Sagittal vertical axis, T1 slope (T1s), T1s-cervical lordosis (CL), anterolisthesis, local kyphosis, the longitudinal distance index, and range of motion were proposed to have relationships with clinical outcomes. The relationship between loss of cervical lordosis (LCL) and T1s has been widely studied, but controversy remains. Extension function, the ratio of CL to T1s (CL/T1s), and Sharma classification were recently proposed as LCL predictors. In predicting postoperative kyphosis, T1s cannot predict postoperative kyphosis, but a low CL/T1s ratio was associated with postoperative kyphosis.
INTRODUCTION
Laminoplasty is an important treatment option for cervical spondylotic myelopathy (CSM) and ossified posterior longitudinal ligament (OPLL) disease. Its long-term clinical and radiological outcomes have also been reported to be excellent [9,21,48,60]. However, some patients have unpredictably poor clinical outcomes after laminoplasty. In this regards, many studies have focused on preoperative sagittal alignment parameters that could predict poor clinical or radiological outcomes. Preoperative cervical kyphotic alignment is the first suggested factor and is also the most important predicting factor for clinical results after laminoplasty [1,58]. The K-line also helped clinicians to predict patients’ clinical prognosis [13]. Recent studies have an interest in the loss of cervical lordosis (LCL) because patients could have a kyphotic alignment or K-line (–) after laminoplasty [19]. In this regard, the T1 slope (T1s) has been spotlighted recently [31]. However, the influx of too many new predictive factors can cause confusion in the analysis of patients’ information [61,63]. In this study, we present an overview of the sagittal alignment parameters that might predict clinical or radiological results through a literature review.
MATERIALS AND METHODS
A comprehensive literature search and analysis was performed using the search terms “laminoplasty” and “alignment” in the Embase and PubMed (MEDLINE) databases for peer-reviewed articles published in English. Articles relevant for this review were selected by the authors if they included information on relationships between pre-operative sagittal parameters and clinical or radiological outcomes.
Since this study aims to analyze the sagittal alignment related parameters, the analysis of the following factors was excluded; differences in the surgical technique (open-door, French-door, C3 laminectomy, and extensor muscle-preserving) [20], surgical devices (sutures, mini-plates, bone grafts, and spacers) [25], the most cephalic level (C3 or C4), and indices using axial images of computed tomography (CT) or magnetic resonance image (MRI), such as space available for the spinal cord [32] and the spinal cord compression ratio [46].
The analyzed parameters were divided into two categories : 1) preoperative radiological parameters predicting clinical outcomes and 2) preoperative radiological parameters predicting radiological outcomes. The radiological outcomes were divided into (2-a) LCL and (2-b) postoperative kyphosis.
RESULTS
We included 32 papers which had focused on pre-operative cervical alignment related parameter to predict clinical or radiological outcomes after laminoplasty. In addition, we searched all references of 32 papers, and nine additional papers related to the subject were identified (Fig. 1) [2,8-10,21,27,48,64,68].
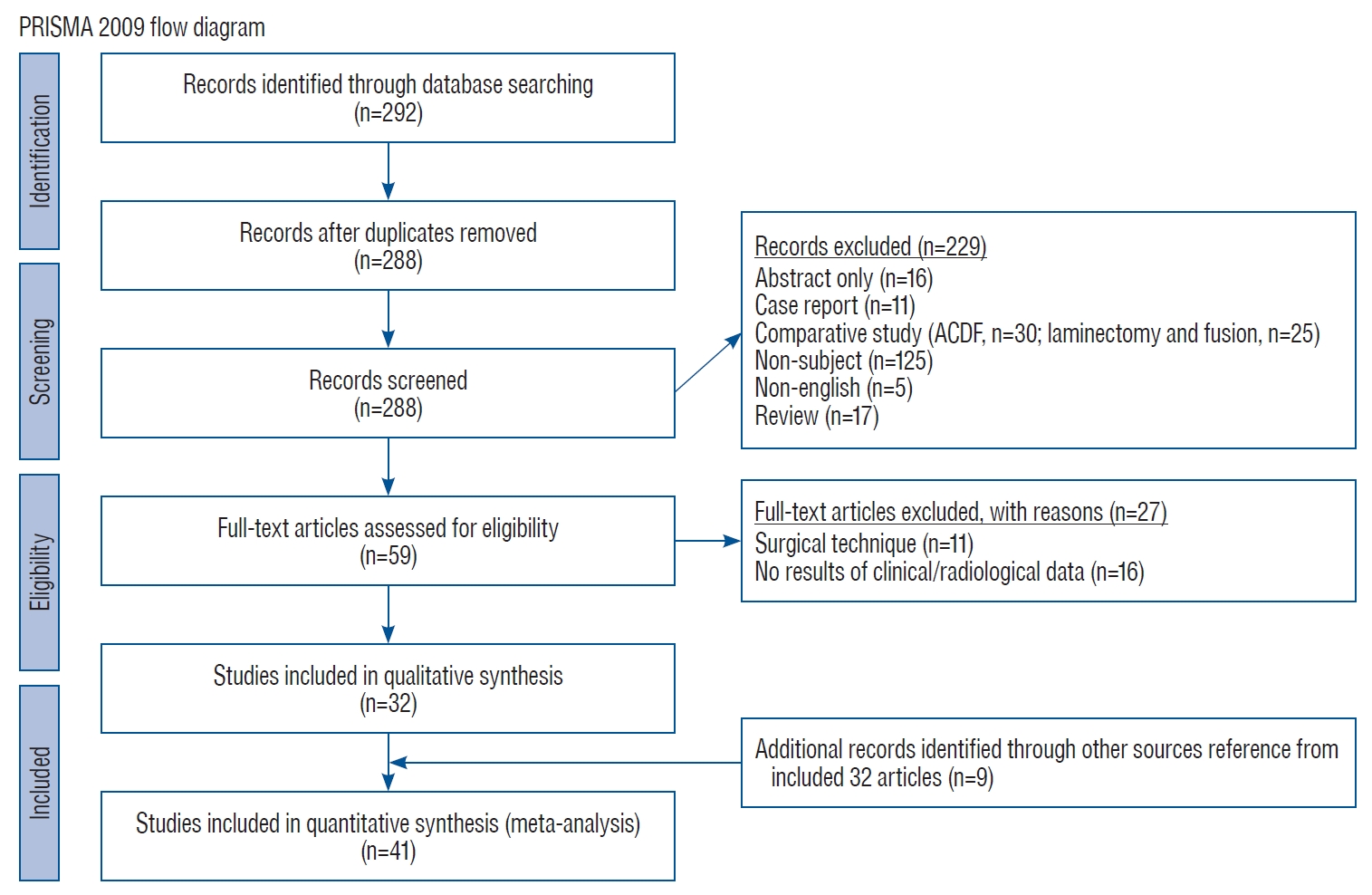
Flow chart diagram of our search mechanism in accordance to the PRISMA. PRISMA : preferred reporting items for systematic reviews and meta-analyses, ACDF : anterior cervical discectomy and fusion.
Pre-operative radiological parameter predicting clinical outcomes
Most of the indices used for outcome measurement were the Japanese Orthopaedic Association (JOA) scale [73] or the modified JOA (mJOA), and the recovery rate (RR) [15] were used. The Visual analogue scale (VAS) of neck pain and the Oswestry disability index (ODI) were also used. The disease entity analyzed in each study is indicated next to the subheading. The included parameters and measurement methods are summarized in Table 1 and Fig. 2. Radiological factors related to clinical outcomes are summarized in Table 2.
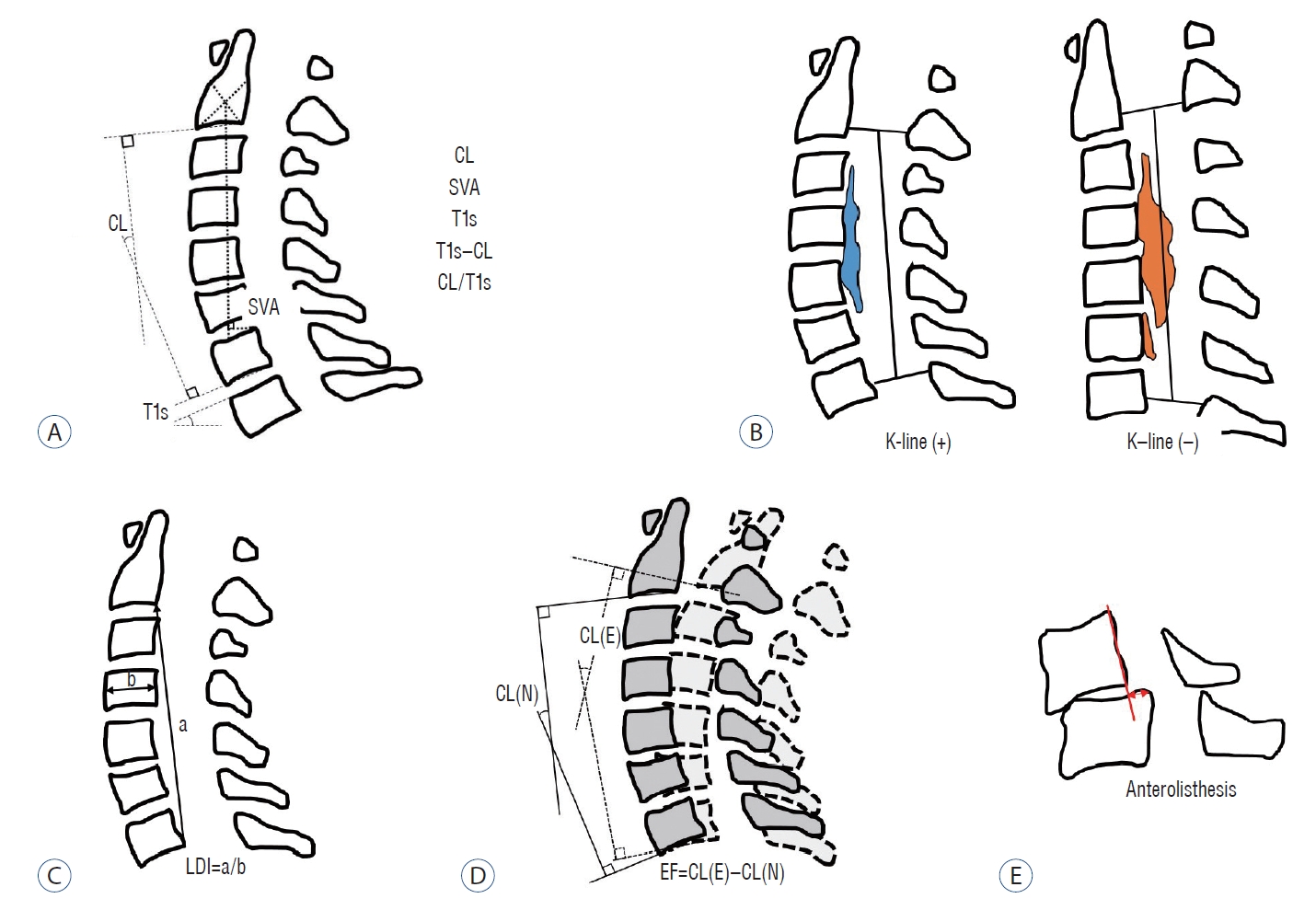
Schematic images of sagittal radiological parameters. A : Routine sagittal parameters. B : K-line. C : a means length of a vertical line drawn between the postero-inferior edges of C2 and C7, b means the antero-posterior diameter of C4, and LDI of the cervical spine. D : Extension function (EF). E : Anterolisthesis in flexion position. CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, LDI : longitudinal distance index, CL(N) : cervical lordosis in neutral position, CL(E) : cervical lordosis in extension position.
Pre-operative kyphotic alignment (CSM and OPLL)
This risk factor was particularly emphasized in laminectomy-only procedures. To obtain a sagittal bowstring effect, preoperative and postoperative lordotic alignment is essential [4,5]. Because laminoplasty preserves more posterior bony structure than laminectomy, it reduces the postoperative incidence of kyphosis, but it cannot change preoperative kyphosis to lordosis [16]. In this regard, it was suggested that patients with preoperative kyphotic alignment should not undergo laminoplasty in order to ensure the sagittal bowstring effect. Baba et al. [2] demonstrated this relationship in laminoplasty through MRI. Posterior cord migration was significantly correlated with preoperative and postoperative cervical spine lordosis. They also found that posterior cord migration was significantly correlated with neurological improvements, and patients with neurological improvement (RR) ≥50% had a significantly larger posterior shift.
However, controversy remains regarding the relationship between preoperative kyphosis and clinical outcomes [12,18,24,30,34,43,47,72]. In a long-term study, Iwasaki et al. [21] included OPLL patients with more than 10 years of follow-up. LCL occurred in 55% of patients, and postoperative kyphotic alignment occurred in 8% of patients. However, preoperative alignment and alignment changes had no significant effects on neurological deterioration. Ogawa et al. [48] also reported no significant difference in the highest postoperative JOA score, RR, or nuchal pain according to preoperative lordotic or kyphotic alignment in OPLL. Additionally, the highest JOA score and RR were not significantly different according to LCL occurrence. Chiba et al. [9] analyzed CSM and OPLL patients with more than 10 years of follow-up. They reported that preoperative alignment did not affect the RR in CSM patients, but preoperative kyphotic alignment tended to be related to a lower RR in OPLL patients.
K-line (OPLL), modified K-line (CSM) and variants
Preoperative alignment is a concept that does not include the size of the OPLL, so it has limitations in predicting clinical results. Fujiyoshi et al. [13] proposed a new index, the K-line, which includes preoperative alignment and OPLL size. They reported that K-line (–) was closely associated with a low RR. A recent study reported that laminoplasty was also effective in patients with K-line (–) in the neutral position, but K-line (+) in the extension position [40].
The concept of the K-line was originally based on lateral images of the cervical spine. It is difficult to measure, especially for patients with a short neck. Ijima et al. [17] pointed out the mismatch between K-line (–/+) in standing lateral images of the cervical spine and supine CT images. Specifically, four of the 33 patients who were measured as K-line (–) on CT images were identified as K-line (+) based on X-rays. Although the clinical results of these mismatched patients were not reported, their findings demonstrate that the K-line cannot be replaced by supine-position images.
Taniyama et al. [68,69] developed a modified K-line (mK-line) using T1-weighted sagittal MRI for CSM. Based on the mK-line, they measured the minimum interval (INTmin) between the mK-line and the anterior compression factor on midsagittal images. In patients with an INTmin <4 mm, significant residual anterior compression of the spinal cord (insufficient indirect decompression) may occur, and an INTmin <4 mm is therefore associated with a lower RR than an INTmin ≥4 mm. The findings of Sun et al. [66] also support the association of the mK-line with clinical outcomes.
Other variants, such as the kappa line [35], K-line tilt [55], coronal K-line, and K-plane [37] have been presented at academic meetings, but no clinical articles have investigated their usefulness.
Sagittal balance-related parameters (CSM and OPLL)
Rao et al. [54] reported that a mismatch of preoperative T1s and cervical lordosis (CL) of more than 20° (T1s-CL ≥20°) was related to poor RR in CSM patients. Sharma et al. [62] classified CSM and OPLL patients into four groups using T1s and the sagittal vertical axis (SVA). They reported that the balanced group (T1s <30° and SVA <20 mm) had good improvements in the ODI, but the unbalanced group (T1s ≥30° and SVA ≥20 mm) had poor ODI improvements. Furthermore, various cut-off values of SVA (28.9, 30, 35, and 50 mm) and T1s-CL (20°) have been reported to be related to clinical results [7,23,51,57].
However, Tamai et al. [67] performed a propensity score–matching analysis adjusting for age, sex, cervical alignment, and preoperative JOA scores. In an analysis of Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire responses based on sagittal balance (SVA, 40 mm), no statistically significant differences according to balance were found.
T1s (CSM and OPLL)
Three studies reported no significant relationship between T1s and clinical outcomes. Miyazaki et al. [47] found that the MR grade was associated with RR in OPLL patients, but T1s was not. Fujiwara et al. [12] also reported no significant relationship between T1s and clinical outcomes in CSM and OPLL patients. Cho et al. [10] similarly reported that T1s was not related to VAS, the neck disability index, or the Short form-36.
Range of motion (ROM) (OPLL)
Maruo et al. [43] found that preoperative alignment, LCL, occupying ratio, and MR T2 high signal intensity were not associated with poor outcomes; instead, only preoperative ROM showed an association with poor outcomes. The odds ratio of an ROM >20° for a poor outcome was 4.853 (95% confidence interval [CI], 1.263–16.635). Masaki et al. [44] also reported that larger preoperative and postoperative ROMs were related to poor outcomes.
Radiological change (LCL, post-operative kyphosis) (CSM and OPLL)
Controversy exists regarding whether these two factors are of clinical significance. Sakaura et al. [57] found that the RR was lower in CSM patients with postoperative kyphosis. This relationship was not found in OPLL patients. Sharma et al. reported that an LCL >10° was related to lower ODI changes [62]. Masaki et al. [44] also reported that greater LCL was associated with poor outcomes. However, other studies have reported that LCL or postoperative kyphosis did not affect clinical outcomes [34,43,47].
Miscellaneous
Anterolisthesis (CSM) was a significant risk factor for poor outcome (p=0.01), whereas retrolisthesis did not affect the neurological outcomes (p=0.6) [50]. Local kyphosis (CSM) was related with poor outcome (RR <50%) (odds ratio [OR], 6.69 per 10° kyphosis; p<0.01) [64]. Longitudinal distance index (LDI) of cervical spine (CSM and OPLL) was significantly lower in the CSM group than in the OPLL group. Also, LDI had a weak but statistically significant negative correlation with RR (r= -0.308, p=0.014) [8].
Preoperative radiological parameters predicting radiological outcomes
LCL
Pre-operative T1s, SVA, CL, ROM, T1s-CL, the ratio of CL to T1s (CL/T1s) and extension function (EF) have been proposed as risk factors for LCL. Table 3 summarizes the relationships of LCL with those proposed factors.
T1s : Kim et al. [31] first reported that high/low T1s were related to LCL in CSM. On the contrary, Cho et al. [10] reported no relationship between T1s and LCL. Subsequently, studies reporting positive or negative findings regarding this relationship have been published [10,38,39]. Even in papers supporting the existence of a relationship between T1s and LCL, the correlation coefficient (r) was low, near 0.3 [27,33,36,47,56,74].
EF : This parameter represents the contraction reserve of the posterior musculo-ligament complex. This factor was found explained the phenomenon of low LCL in patients with a high T1s. Lee et al. [39] reported that the correlation coefficient (r) between EF and LCL was 0.504, which had a stronger correlation than that found for T1s. This parameter is also included in the Sharma classification [62].
Ratio of CL to T1s (CL/T1s) : Li et al. [41] classified the CL/T1s ratio as low (bottom 25%; CL/T1s <0.45), fair (middle 50%; CL/T1s ranging from 0.45 to 1.05), or high (top 25%; CL/T1s >1.05). A high CL/T1s ratio was significantly related to a high LCL (high ratio, 14.53±0.63; fair ratio, 5.51±7.59; low ratio, 0.95±9.84; p<0.001).
Sharma classification : The Sharma classification presents a scoring system including preoperative CL, T1s, and EF [62]. Of particular note, it separately presents straight curvature (Cobb angle [CA] <10°), which can frequently occur in patients with postoperative kyphosis due to LCL. In the score 0 group (CA <10°, T1s <30°, EF >12°), significant LCL (>10°) occurred in 0% of patients. In contrast, 100% of patients with a score of 4 (CA >10°, T1s >30°, EF <12°) had significant LCL.
Postoperative kyphosis
Postoperative kyphosis is a distinct concept from LCL. In postoperative kyphosis, LCL occurs on the basis of preoperative CL, and as a result, the postoperative CL is <-10°.
Preoperative CL <10° : Patients with preoperative CL <10° can easily develop postoperative kyphosis, even with a slight LCL. Suk et al. [65] reported that patients with preoperative CL <10° had more postoperative kyphosis than those with preoperative CL >10° (OR, 7.625; p=0.008).
Kyphotic angle in flexion position > lordotic angle in extension position : This pattern was related to postoperative kyphosis (OR, 9.167; p=0.005) [65].
T1s : Three studies analyzed the association between high/low T1s and postoperative kyphosis, but found no significant association between the two factors [27,31,47].
CL/T1s : Patients with a low CL/T1s ratio had a significantly higher rate of postoperative kyphosis than those with a fair or high ratio (OR, 16.63; 95% CI, 3.07–90.12; p<0.001) [41].
Case presentation
We categorized the preoperative alignment parameter for which laminoplasty is relatively preferred or not through a review of the previous literature (Fig. 3). In patients with straight or lordotic curves, LCL prediction is important. If the risk of LCL is low, sufficient decompression can be expected (case 1), but if the risk of LCL is high, postoperative alignment could be changed to kyphotic alignment (CSM) or K-line (–) (OPLL) (case 4). These changes closely related to insufficient decompression, leading to a poor clinical outcome. In the case of kyphotic alignment, laminoplasty corresponds to relative contraindication (case 3). However, as reported in the previous literature, some patients recovered to lordosis after surgery, and have shown a relatively good clinical course [9,21,48]. There is no known mechanism about the recovery of kyphotic alignment to the lordotic curve after surgery, but we should note that patients with kyphotic alignment could be compensatory alignment due to pain limitation (case 2). The extension position helps to differentiate these compensatory alignments. This differentiation can help determine whether to perform laminoplasty in kyphotic alignment patient group with a high risk of complications from the fusion operation, such as elderly and severe osteoporosis.
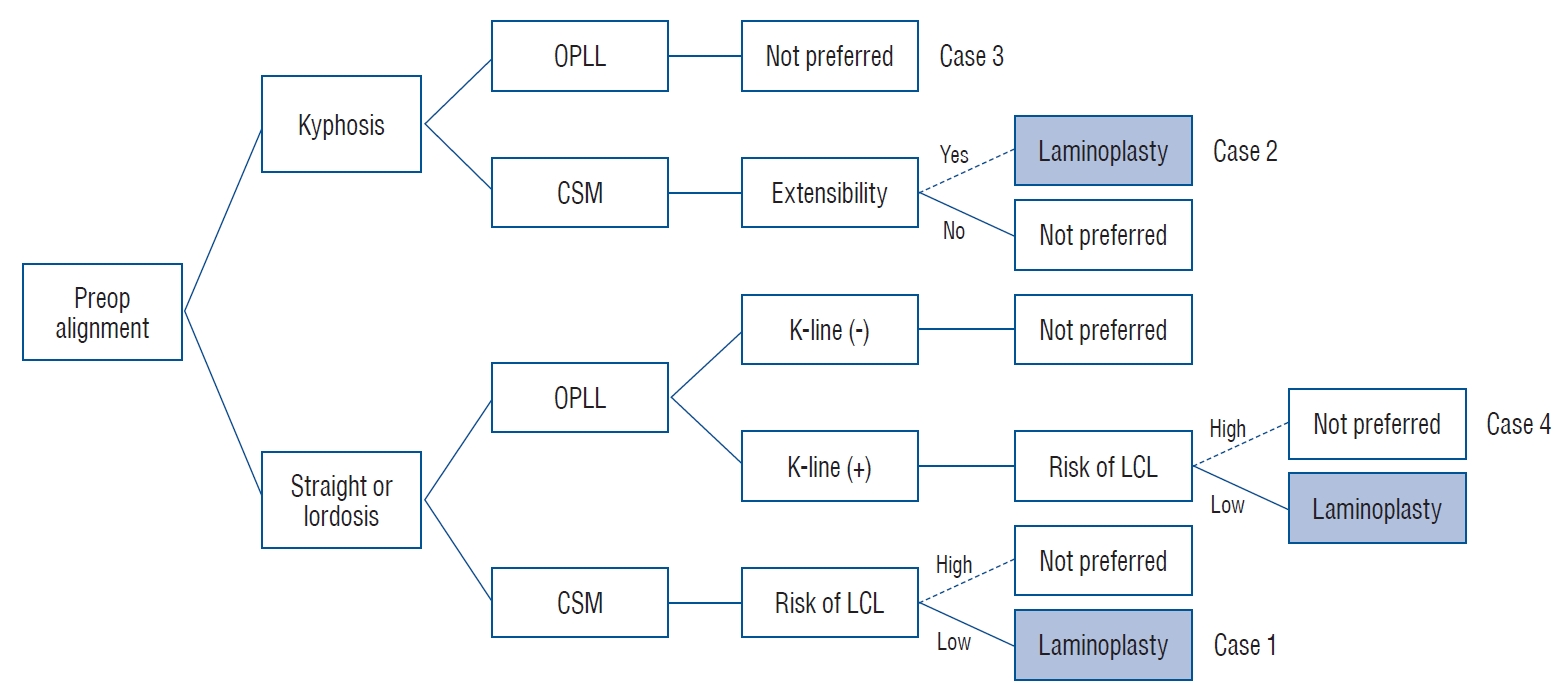
Schema of the indication of laminoplasty according to preoperative alignment, diagnosis, K-line, and loss of cervical lordosis. Preop : preoperative, OPLL : ossified posterior longitudinal ligament, CSM : cervical spondylotic myelopathy, LCL : loss of cervical lordosis.
Case 1 (Fig. 4)
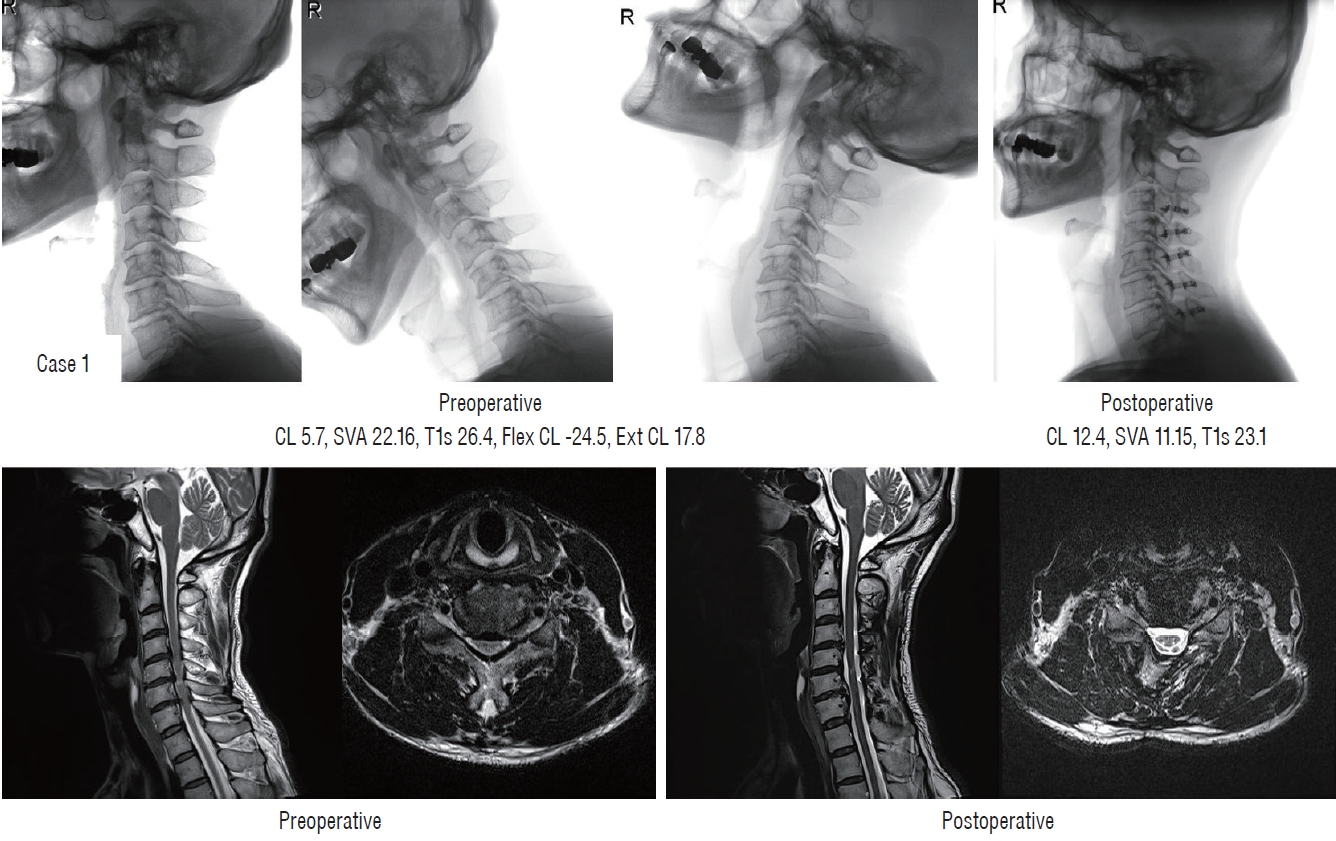
Sufficient indirect decompression (case 1). CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, Flex CL : cervical lordosis in flexion position, Ext CL : cervical lordosis in extension position.
A 55-year-old male patient with preoperative straight curve had severe preoperative neck pain (VAS, 7), and gait disturbance (pre-operative mJOA, 15). Preoperative CA was 5.7°, T1s was 26.4°, and EF was 12.1°. This corresponds to ‘Ia’ type and score 0 in Sharma classification and the probability of LCL was reported as 0%. Postoperative CA was 12.4° and no LCL occurred. After surgery, neck pain was decreased (VAS, 4), and mJOA recovered to 18 (RR, 100%). On postoperative MRI, we found that the spinal cord was freed from the anterior lesion by indirect decompression following sufficient posterior shifting after laminoplasty.
Case 2 (Fig. 5)

Different postoperative alignment and clinical outcomes in two patients with preoperative kyphotic alignment (case 2 [upper] and case 3 [lower]). CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, Flex CL : cervical lordosis in flexion position, Ext CL : cervical lordosis in extension position, EF : extension function.
A 66-year-old male patient had a preoperative kyphotic alignment (preoperative CA, -15.9°; T1s, 15.2°; EF, 25.60°). The patient had severe preoperative arm pain (VAS, 8) and complained of a decrease in hand fine motor and gait disturbance (preoperative mJOA, 12). Although kyphotic alignment was not applied to Sharma classification, both T1s and EF were low-risk factors for LCL. The patient recovered to straight curvature (postoperative CA, 0.9°) after surgery. The neck pain did not improve, but the arm pain improved. (VAS, 3), and mJOA recovered to 16 (RR, 66.7%).
Case 3 (Figs. 5 and 6)
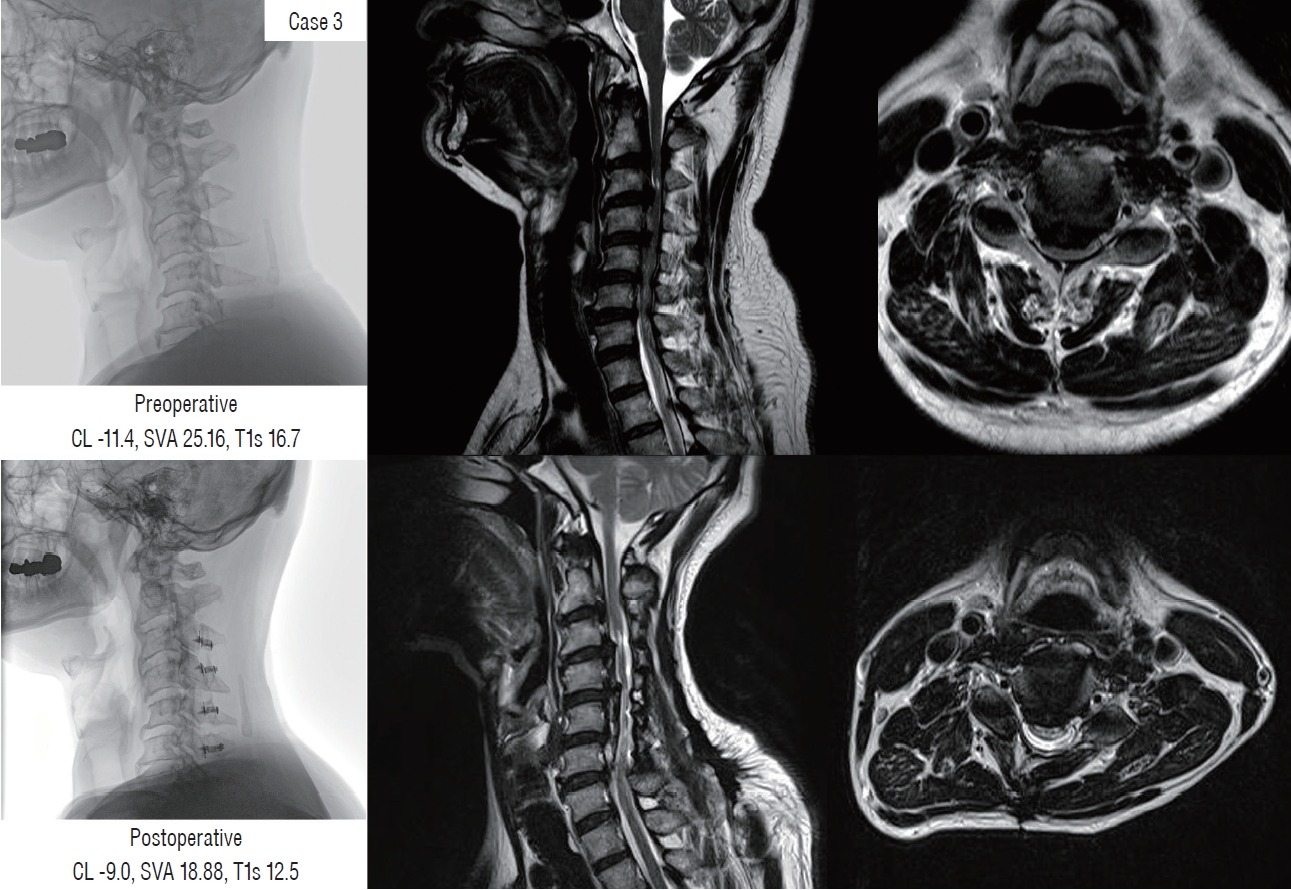
Failure of indirect decompression in patients with preoperative kyphotic alignment (case 3). CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope.
A 52-year-old male patient was diagnosed with C2–6 continuous type OPLL. The patient complained of severe neck pain and arm pain (both VAS, 8), deterioration of the hand fine motor and gait disturbance (preoperative mJOA, 10). The patient had a preoperative kyphotic alignment (preoperative CA, -11.4°), and the EF was also limited to 7.1°. There was no significant change in alignment after surgery (postoperative CA, -9°) and T1s was decreased for compensation (preoperative, 16.7°; postoperative, 12.5°). Neck and arm pain partially decreased (neck VAS, 6; arm VAS, 4), but there was no significant improvement in hand fine motor and gait (mJOA, 13; RR, 37.50%). On postoperative MRI, the spinal canal was widened after laminoplasty, but the cord was still compressed by the anterior lesion.
Case 4 (Fig. 7)

Failure of indirect decompression following loss of cervical lordosis in preoperative straight alignment patients (case 4). CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, Flex CL : cervical lordosis in flexion position, Ext CL : cervical lordosis in extension position, EF : extension function.
A 52-year-old male patient with segmental OPLL complained of severe arm pain (VAS, 7) and fine hand motor weakness (mJOA, 15). The patient had a preoperative straight alignment (preoperative CA, -1.4°), Preoperative T1s was 18.0°, and EF was 10.6°. This corresponds to ‘Ib’ type and score 1 in Sharma classification, and the probability of LCL was reported as 20%. There was 11.8° of LCL, and kyphotic alignment was obtained after surgery (postoperative CA, -13.2°). We found the insufficient indirect decompression in postoperative MRI. There was some improvement in arm pain after surgery (VAS, 4), but there was no significant improvement in fine motor weakness (mJOA, 16; RR, 33.3%).
DISCUSSION
The World Federation of Neurosurgical Societies (WFNS) spine committee recently announced recommendations for CSM and OPLL [3,11,53,75-77]. The WFNS recommendations pointed out that the most important factors associated with the clinical results of CSM are age, symptom duration, and disease severity. However, because these factors are non-modifiable, numerous studies have attempted to find modifiable factors that influence clinical outcomes. The most important modifiable factor related to clinical results is the surgical approach [14,52]. Among the several surgical approaches, laminoplasty is preferred because it has fewer complications than anterior corpectomy and fusion or posterior laminectomy and fusion, especially in older osteoporotic patients [3,14,28,40,71]. The current consensus is that laminoplasty is indicated in patients with neutral or lordotic alignment without significant axial pain and in K-line (+) OPLL patients. However, these indications do not always lead to good clinical outcomes. This review conducted a literature review of all possible pre-operative radiological parameters on why poor clinical/radiological outcomes occur in some of the patients even corresponding to the indication.
Most studies investigating the effect of preoperative alignment on clinical outcomes did not report statistical significance (Table 2). The clinical results are primarily affected by age, disease severity, and symptom duration. Additionally, MR-based parameters, such as the occupying ratio, OPLL shape, and cord signal change have a significant impact on clinical outcomes. Complications of laminoplasty such as LCL, C5 palsy [49], postoperative neck pain, increased size of OPLL [70], decreased ROM, and insufficient decompression also affects clinical outcomes. In this regard, there is a limited degree to which clinical effects can be analyzed in terms of alignment factors alone. Various factors are involved in predicting clinical outcomes, and further research using recent big data technology (e.g., deep learning) is needed for a comprehensive analysis [22,26,29,59].
Patients with alignments suitable for laminoplasty can proceed with postoperative kyphotic alignment or postoperative K-line (–) according to LCL. In this regard, LCL has been actively studied, but the exact mechanism has not been established. Many studies have investigated the role of T1s in LCL, but the reported correlation coefficients are low (near 0.3), and some studies have also reported no correlation (Table 3). A meta-analysis is needed to resolve this controversy. Recognition of the limitations of T1s as an LCL predictor led to the study of new risk factors, such as EF, CL/T1s, Sharma classification. EF is a recently proposed factor that showed a higher correlation coefficient than existing factors [39]. The correlation between LCL and EF was also confirmed by Sharma et al. [62]. Li et al. [41] reported more LCL was related to high CL/T1s, and postoperative kyphosis was related to low CL/T1s. The Sharma classification has shown an excellent prediction rate of significant LCL. However, reproducibility studies in other groups have not yet been conducted, and the Sharma classification does not reflect differences among disease entities, such as CSM and OPLL.
This study has the following limitations. First, this study was aimed at systematic review, but nine additional papers were identified in the reference during the searching process (9/41, 22%). The influx of these additional papers can act as a limit to securing objectivity as a systematic review. The second, we did not perform meta-analysis related to outcomes. This study focuses on the identification of various factors. In that respect, many factors have been suggested, and various clinical or radiological factors have been suggested as dependent factors. In that respect, there was a limit to performing a meta-analysis.
CONCLUSION
Numerous sagittal parameters are associated with clinical and radiological outcomes after laminoplasty. We classified the suggested sagittal parameters into clinical and radiological results and summarized the previous literature. Pre-operative kyphotic alignment, K-line, and pre-operative sagittal balance were considered important factors in the prediction of clinical results. In addition, we should pay attention to the occurrence of postoperative kyphotic alignment according to LCL even without preoperative kyphotic alignment. With regard to LCL, T1s has been suggested as an important risk factor. However, due to the weak correlation between T1s and LCL, new factors, such as EF, CL/T1s, and Sharma classification, have been proposed, and validation of these factors is required.
Notes
CONFLICTS OF INTEREST
Dong Wuk Son has been editorial board of JKNS since November 2017. He was not involved in the review process of this original article. No potential conf lict of interest relevant to this article was reported.
INFORMED CONSENT
This type of study does not require informed consent.
AUTHOR CONTRIBUTIONS
Conceptualization : DWS, JJS, YH, GSS
Data curation : SHL, DWS, JJS, JSL
Formal analysis : SHL, DWS, JSL
Funding acquisition : SHL, DWS, JSL, GSS
Methodology : SHL, DWS, JJS, YH, GSS, SWL
Project administration : SHL, DWS, JJS, YH, GSS, JSL, SWL
Visualization : SHL, DWS, JJS, JSL
Writing - original draft : SHL, DWS, JJS, YH, GSS, JSL, SWL
Writing - review & editing : SHL, DWS, JJS, YH, GSS, JSL, SWL
Acknowledgements
This study was supported by Research institute for Convergence of biomedical science and technology (30-2018-020), Pusan National University Yangsan Hospital.



