Perioperative Results and Complications after Posterior Lumbar Interbody Fusion for Spinal Stenosis in Geriatric Patients over than 70 Years Old
Article information
Abstract
Objective
As increasing the size of the geriatric population, the number of elderly patients, who need the surgery for painful degenerative spinal stenosis has been increasing. The geriatric population may be relatively high complications, because of age and age-associated medical conditions. However, there is a lack of studies addressing the perioperative complications and outcomes in elderly patients with posterior lumbar inter body fusion with screw augmentation (PLIF).
Methods
We retrospectively reviewed the medical records and radiographic studies of geriatric patients who had spine surgery of PLIF due to spinal stenosis for 11 years. We divided into 2 groups (A; 70–75 years, B; over then 76 years) according to the age. Surgical level of each groups, hospital day and postoperative day, co-morbidities, complications, clinical outcomes were analyzed. Operative reports, hospital and outpatient clinic charts, and radiographic studies were reviewed.
Results
Group A was composed of 80 patients, their mean age was 72.21 and female dominant (n=46), and their mean surgically fused level was 1.52 level. Group B was 36 patients, their mean age was 78.83 and female dominant (n=20), and their mean surgically fused level was 1.36 level. Comparing between two groups, complications, postoperative hospital stay were slightly increase in group B and co-morbidity was statistically high in group B, however clinical outcomes were similar between two groups.
Conclusion
Increasing age might be an important risk factor for complications in patients undergoing PLIF, however, we would like to recommend that if the situation of spine of extreme geriatric patients need PLIF, it should be in the surgeon’s consideration after careful selection and clinical judgement.
INTRODUCTION
Aging is a natural process and is known for reduction in regeneration and repair of cells as time passes due to physical and mental alteration16). Degenerative spinal diseases from such aging are major anatomical structural changes and are mostly defined as diseases that compresses nerve roots due to stenosis in spinal canal or intervertebral neural foramen after degenerative changes in dynamic segment11,12).
In these times when various changes like development of medicine and improvement in social environment lead to increased life expectancy, increased number of patients suffer from degenerative lumbar spondylosis7,16). Therefore, older patients require not only standard drug treatment and conservative treatment, but furthermore a treatment that reflects quality of life. However, when considering surgical treatment for patient diagnosed with spinal stenosis, important factor in deciding level of treatment is age.
Numerous studies have continuously reported higher rate of complications in older patients after surgical treatment8,12,14,23,28). A study of patients aged 75 and older who underwent decompressive spine surgery reported a much higher complication rate (35.2%), and it contains a major complication rate of 12.5%8). Therefore, when we decide the therapeutic range of older patients who suffered from spinal stenosis, surgical treatment was hesitant due to relatively high complication rate13).
However, in contrast, there have been numerous reports that older spinal stenosis patients have no difference in post-surgical complication or clinical outcome compared with younger patients24,25,31,33,36). Various techniques are globally being performed for surgical intervention on lumbar spinal stenosis and minimal invasive surgery, depressive surgery, and spinal fusion are universally practiced17,22,34). However, most of those studies are based on patients who have received decompressive surgery as subjects15,18,20,33,34).
Therefore, the goal of this study lies in evaluating whether posterior lumbar interbody fusion with screw augmentation (PLIF) is appropriate for elderly patients aged over 75 after comparing clinical result and complications in different age groups of patients aged 70 or more.
MATERIALS AND METHODS
Patient population
This study is based on patients aged 70 or more who have received posterior lumbar fusion with pedicle screw fixation between January 2006 and December 2016 after being diagnosed with lumbar stenosis. Among 126 patients who have received fusion surgery, 116 patients, excluding 10 patients who met criteria for exclusion, have been divided into the group A with 80 patients aged from 70 to 75 and the group B with 36 patients aged more than 75 and evaluated for complication and outcome. For precise evaluation of spinal fusion outcome in degenerative spinal disease, patients who have received fusion surgery from diseases other than degenerative spinal disease have been excluded. Exclusion criteria are as following: 1) patient who only have performed decompressive surgery; 2) patient diagnosed with spinal stenosis due to metastatic or spinal tumor; 3) Patient diagnosed with spinal stenosis due to trauma; and 4) infectious spinal disease.
Radiologic evaluation
Diagnosis of spinal stenosis was based on clinical symptoms, physical examination of neurology, simple lumbar spine x-ray, lumbar magnetic resonance image, lumbar computerized tomography. All patients were conducted of conventional PLIF by single surgical team. After surgery, simple lumbar spine x-rays were obtained in 1 month, 3 months, 6 months, and 1 year. Successful spinal fusion was evaluated based on lumbar dynamic x-ray obtained 1 year after the surgery. Complete fusion was defined as 1) incorporation of grafts on both endplates; 2) presence of bridging trabecular bone across the interspace; 3) <2-degree movement on lateral flexion/extension views; and 4) absence of graft migration and subsidence2).
Pre-operative evaluation
All patients were recorded of past medical history and co-morbidities in medical record before surgery and preanesthetic evaluation was performed by our anesthesiologist. Anesthesia risk was evaluated based on American Society of Anesthesiologists (ASA) score. Clinical symptom of patients was estimated by Visual Analog Scale (VAS) score for back pain and lower extremity radicular pain.
Post-operative evaluation
Surgical level, hospital day, post-operative admission day, clinical symptom change, complication, postoperative outcome, radiologic and clinical evaluation were perfomed. Postoperative complications were further classified as major and minor complications following the literature which had been reported in 2008 by Cloyd et al.8). Major complication was defined as adversely affecting the recovery of the patient and minor complication was defined as recorded in the medical chart but did not alter the recovery of the patients.
Statistical method
Statistical analysis in this study was conducted with SPSS for Windows (version 21.0; SPSS Inc., Chicago, IL, USA). Statistical significance was established with p value of less than 0.05.
RESULTS
Patient population
Average age was 72.71 in group A of 70–75 and 78.83 in group B over 75, with the oldest being 89. Number of surgical treatment level was 1.52 for group A and 1.36 in group B, but it did not show statistical significance (p=0.142, Table 1).
Pre-operative evaluation
Number of co-morbidities in the patients was 125 in group A and 70 in group B. A group had average co-morbidities of 1.56 while B group had 1.94 and it has been evaluated that group B had more statistically significant co-morbidities (p=0.038). In ASA score performed as pre-operative anesthetic evaluation, A group showed average of 2.23 (0–3), while older group showed 2.3 (1–4). With older age, pre-operative risk was higher, but it was not statistically significant (p=0.258).
The most common co-morbidity was hypertension and patients might have diabetes, history of stroke, ischemic heart disease, chronic kidney disease, lung disease, and tumor or cancer (Table 2). Hypertension was most common in both groups and diabetes was more prevalent in older age group, with 32.5% in old group and 47.2% in older group.
As for VAS score on lower back pain and lower extremity radicular pain evaluated as pre-operative clinical symptom, group B showed higher score of lower back pain than group A, whereas pain from the radicular pain was higher in group A (Table 3).
Post-operative evaluation
Post-operative complications
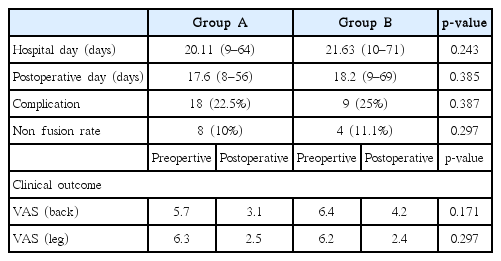
In group A, 18 (22.5%) post-operative complication occurred and 9 (25%) complications occurred in 36 patients of group B. Post-operative complications were a slightly higher in group B, but there was no statistical difference between two groups. The most common complication was post-operative infection in both groups, and 2 cases of post-operative hematoma in surgical region occurred in group A. Also, there were major complications like pneumonia and stroke. In group B, 3 patients (8.3%) occurred major complications and it is slightly higher rate than group A with 3 patients (3.75%). However, there was no statistically significance. In addition, complications such as urinary tract infection, acute renal failure, leukopenia, post-operative delirium occurred (Table 4).
Clinical & radiographic outcomes
In dynamic lumbar x-ray performed 1 year after the surgery, 8 (10%) in group A, and 4 (11%) in group B was evaluated as failure in bone fusion. Average hospital day and post-operative day were higher in group B than group A, but it was not statistically significant. Both groups showed decrease in VAS score for lower back pain and lower limb radicular pain. Most patients showed high satisfaction after surgery.
DISCUSSION
With global increase in life expectancy, the number of elderly patients with painful degenerative spinal stenosis requiring surgery is expected to rise. Degenerative spinal disease is prevalent in geriatric population and age is an important factor in deciding technique of surgery and its extent1,3,28,36). Numerous studies have reported that post-operative complication is higher in old patients than younger patients9,12,16). In a 2007 literature published by Daubs et al.12), when patient aged 60 or more with spinal deformity received surgical treatment, 37% of the patients showed complication and percentage of serious complication such as pneumonia and stroke was 20%. This is exceptionally high from 16.4% reported by a study of 2010 by Nasser et al.30). that included 79417 patients who received surgery for degenerative spondylosis, which it is agreeable that age increases risk of post-operative complication. In our study, 25 patients of total 116 patients (21.5%) underwent PLIF surgery showed post-operative complications, and 16 patients (20%) were group A, 9 patients (25%) were group B. It was similar results with complication rates of other literatures.
In contrast, many studies report risk of post-operative complication in elderly patients is similar to that of young patients27). In a large-scale retrospective cohort study with 2320 patients by Saleh et al. 33), among old patients in age 80 or older who received lumbar spine surgery, 16.34% showed post-operative complication and 3.23% showed serious complication. Such result is similar to the data of complication rates after spinal surgery that described Nasser et al.30), 2010, which it makes surgical treatment to be a valid option for patients in old age. Also, Rihn et al.31), 105 patients aged 80 or older who were diagnosed with spondylolisthesis and spinal stenosis and performed surgical treatment showed complication risk and mortality similar to young patient.
Furthermore, Cloyd et al.9) stated age alone is not determinant for avoiding surgery in patient with spinal disease. In other literature, low body weight (body mass index <18.5) was reported to be a crucial factor in predicting readmission of patient after surgery25,33). Other than age and body weight, the fact that diabetes increases risk of complication after surgery is known from various literatures21,26). Gruskay et al.23) suggested bone fusion segment decides admission period and post-operative hospital day. In our study, there was no single important factor affecting the higher complication rates. Even co-morbidity was higher in group B than group A, but there was no significant difference in complication rates between two age group.
Outcome of surgical treatment in old-age patients with spinal disease is being reviewed positively in various papers. However, there are controversies on outcome and complication of minimal invasive surgery, decompression-only surgery, and intervertebral fusion4,6,14,29,32,37). Epstein15) reported surgeons prefer bone fusion in younger patients and when only decompressive surgery was performed, it showed similar improvement of symptoms as patient who received interbody fusion and the surgery can decrease complication of interbody fusion from hemorrhage during surgery and longer operation time. Furthermore, Dagistan et al.11) insisted that 37 patients age from 65 to 86 who received minimal invasive decompressive surgery would be expected of significant improvement in quality of life.
However, there have been objective reports that PLIF is necessary for patients who progressed spinal instability after decompressive surgery5). According to the paper by Glassman et al., lumbar interbody fusion can be considered as option for patients age 65 or older and post-operative complication does not influence clinical results22). Coric and Branch10) reported that decompression-only surgery had failure risk of 30–40% in patients with symptomatic spinal stenosis and 10–20% of the patients came to have revision surgery. Also, they argued that instability may occur in patients who received decompression-only surgery, risk of lower back pain may be decreased, and post-operative complication is similar17,19,25,35).
This retrospective study showed post-operative improvement of symptom and complication rate in elderly patient group aged over 75 who had similar surgery to patient group A in 70–75. Though group B showed significant increase in co-morbidities, but there was no significant difference in post-operative outcomes. Also, this study can be considered to have its significance in that it excludes patients who only had decompressive surgery and only selects old patients who have received PLIF as subjects. Degenerative change of spine is natural aging process and there were much more patients with spinal stenosis than only herniated intervertebral disc patients in elderly people. Even there is still controversial, concomitant fusion surgery after decompression has numerous benefits compared with only decompressive surgery especially, spondylolisthesis patients. Our study showed similar complication rates between group A and group B in spite of more medical co-morbities in group B. This results support performing PLIF surgery with elderly spinal stenosis patients. Therefore, it is suggested that surgeon will consider comparatively more invasive surgery in old patients aged 76 or older in deciding the extent of surgery.
However, this study has a disadvantage that it cannot be free of selection bias in a retrospective study and has limitation of comparatively irregular follow-up period and the fact that the outcomes are evaluated from only one surgical team.
CONCLUSION
Age is an important factor in deciding extent of surgical treatment in patients with spinal disease. Though there are controversies, it should be considered carefully as aging, itself, is risk of increasing post-operative complication risk. Many literature support higher post-operative complication risk of geriatric patients who undergone spinal surgery and it contains major complications such as stroke and pneumonia. However, as shown in the outcome of this study, older patients aged over 75 show significantly higher risk of comorbidities than patients in 70–75, there is no statistically difference in post-operative complications and outcomes. It might be allowed various surgical treatment options to spinal stenosis patients who are refractory to conservative management. Also, comparatively invasive treatment like interbody fusion can be a valid option, depending on medical and physical status of individual patient.