Skull Metastasis of Gastric Gastrointestinal Stromal Tumor Successfully Managed by Surgery
Article information
Abstract
Gastrointestinal stromal tumors (GISTs) are rare, but are the most common mesenchymal neoplasm of the gastrointestinal tract. The most common sites of metastasis are liver and peritoneum, while bone metastasis is rare. We report on a patient with skull metastasis after seven years of treatment with imatinib for metastatic GIST. She underwent metastasectomy consisting of craniectomy with excision of the mass, and cranioplasty and continued treatment with imatinib and sunitinib, without evidence of cranial recurrence. She died of pneumonia sepsis one year after metastasectomy. Skull metastasis of GIST is a very rare presentation, and an aggressive multidisciplinary approach should be considered whenever possible.
INTRODUCTION
Gastrointestinal stromal tumors (GISTs) are rare, but are the most common mesenchymal neoplasm of the gastrointestinal tract, with an incidence of 10–20 cases per million7).
These tumors can arise from anywhere in the gastrointestinal tract, and are thought to originate from interstitial cells of Cajal. The stomach is the most common site of origin (60–70%), and the small intestine (20–25%) and the large intestine (5–10%) are other usual sites7). It can present as localized disease, however, metastasis at presentation occurs in up to 50% of cases. In addition, localized disease can recur even after curative surgery. The most common sites to which gastrointestinal tumors metastasize are liver and peritoneum, while lung, bone, or lymph node metastases are rare13). Surgical removal is the only curative option for localized GIST. In cases of metastasis, systemic treatment is a main treatment modality. Before the imatinib era, there was no effective systemic treatment and survival of patients was usually poor. Discovery of a gain-of-function mutation in the c-kit protooncogene in GIST and development of imatinib, a tyrosine kinase inhibitor against the mutation, resulted in a dramatic change of the prognosis of this disease13). As a consequence, median overall survival for metastatic GIST in the imatinib era is approximately five years14). Due to introduction of very effective target agents, we now encounter metastases of GIST, which used to be regarded as unusual sites of metastasis.
Here report on a patient with skull metastasis of GIST after seven years of imatinib treatment who underwent successful metastasectomy.
CASE REPORT
Ten years before the skull metastasis occurs, a 50-year old female patient complaining of dyspepsia was diagnosed with a GIST on the high body posterior wall of the stomach. She underwent gastrectomy, and complete resection of the tumor without rupture was accomplished. The tumor measured 9×7×6 cm in size with a mitotic rate of 52/50 high power field (HPF), less than 10% of necrosis, clear resection margin, and no lymph node metastasis. On immunohistochemical (IHC) staining, CD34 and c-kit were positive, while smooth muscle actin (SMA) and S-100 were focally positive. At that time, neither mutation analysis nor adjuvant imatinib treatment was a routine practice; therefore, she was followed-up with regular examination with out adjuvant treatment.
Nine years before the skull metastasis occurs, recurrence was observed in the abdominal wall and peritoneum. She started 400 mg/day of imatinib, and very good partial response (PR) was achieved and maintained. Although recurred GIST responded well to imatinib, she was suffering from grade 3 anorexia and lethargy, therefore, she took imatinib intermittently. The tumor grew during the imatinib-off period, but shrank again when she resumed imatinib treatment.
Her tumor was under control for seven years, until the peritoneal mass in the right lower quadrant showed progression and invasion of adjacent small bowel and ascending colon. She underwent debulking surgery (small bowel resection and reanastomosis, right hemicolectomy), and the mass measured 11×8 cm in size with 10–13/50 HPF and positive radial resection margin. After surgery, no gross mass was observed; how ever, the dose of imatinib was increased to 600 mg/day. Approximately 16 months later, she found a lump on her head. The mass continued to grow, and CT scan of brain and abdomen which were taken three months later showed a large mass located in the parietal cranial vault suppressing adjacent brain and a small single liver metastasis (Fig. 1). Subsequent MRI revealed a heterogeneously enhancing mass of approximately 7.7 cm ex tent involving the right parietal bone, parietal scalp, and parietal convexity with a heterogeneous signal intensity on a T1/T2 weighted image, multiple signal void on a T2 weighted image, and fatty marrow signal loss with enhancement (Fig. 1). She underwent craniectomy with excision of the mass, cranioplasty, and hepatic resection. On surgical field, about 10×10 cm sized yellowish, relatively soft mass originating from skull was com pressing dura and brain parenchyma. Because mass adhered to the dura and invasion with seeding was grossly suspected, the bone, tumor, and dura were removed as a unit. Diagnosis of metastatic GIST was confirmed by pathologic examination (Fig. 2). She experienced left hemiparesis postoperative day 1, and CT scan indicated intracerebral hemorrhage in the right temporoparietal lobe. This delayed subcortical hemorrhagic trans formation was thought to result from drainage vein sacrifice during the operation. After conservative management and re habilitation, she recovered and was discharged from the hospital. Because the role of adjuvant radiotherapy for GIST is not established, we did not administer adjuvant radiotherapy. In stead, her imatinib dose was elevated to 800 mg/day thereafter, which she was not able to tolerate. After three months of rest, huge masses were found in the liver and peritoneal cavity. There was no recurrence in the cranium. She started sunitinib treatment 6 months after metastasectomy. Unfortunately, she was not able to tolerate sunitinib due to nausea and fatigue; there fore, after 1.5 month of sunitinib treatment, she rested for three months. As the masses progressed, she resumed sunitinib, when 1 year has passed since metastasectomy. A month after sunitinib resumption, she was admitted to the hospital via the emergency department for fever and dyspnea, and diagnosed with pneumonia. She died of acute respiratory distress syndrome one month later, when 14 months has passed since skull metastasectomy.
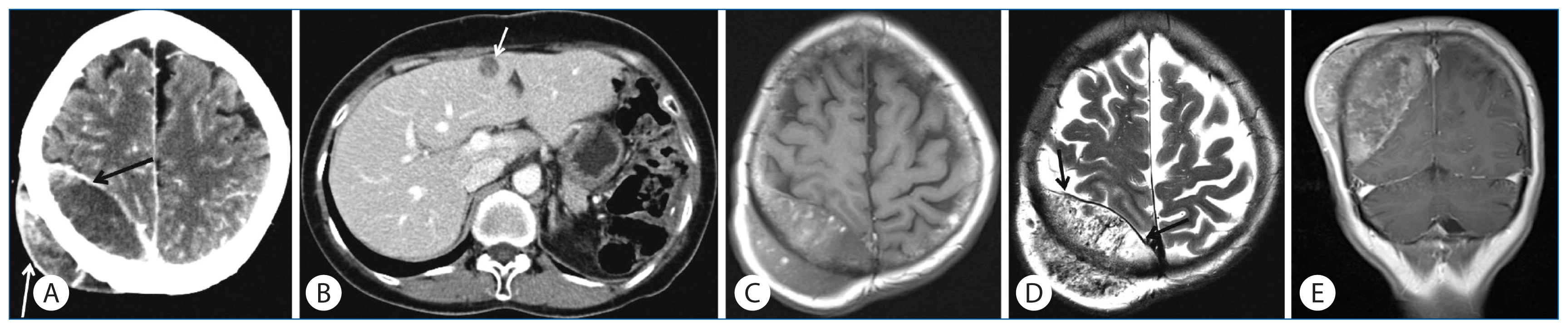
Imaging findings of skull metastasis and hepatic metastasis in a patient with malignant gastrointestinal stromal tumor. A: Post-contrast brain CT image reveals a 7.7 cm sized, well-defined mass (arrows) centered on the diploic space of the calvaria. B: Abdomen CT image reveals a hypodense single metastasis (arrow) in left medial segment of the liver. C and D: Axial T1- (C) and T2-weighted (D) MR images show heterogeneous signal intensity of the skull metastasis. The dura (arrows) is intact and the underlying cortex appears compressed. Note the multiple signal voids on T2-weighted image. E: After gadolinium enhancement, the mass demonstrates heterogeneous enhancement.
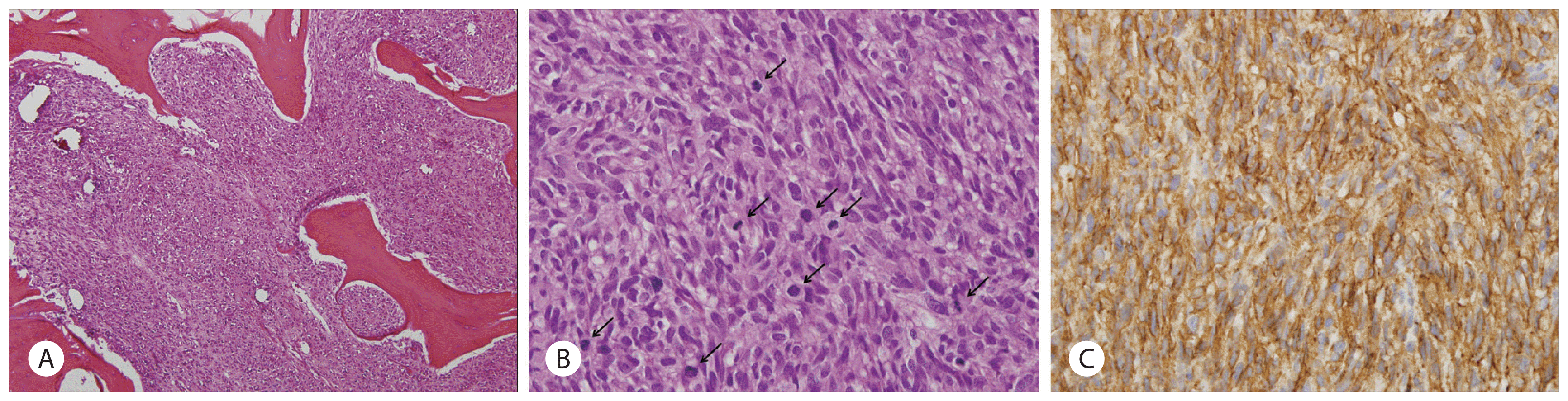
Pathology of a resected skull tumor. A: Metastatic gastrointestinal stromal tumor in the skull. The tumor consists of atypical spindle cells with high cellularity and infiltrative growth pattern with destruction of normal bone tissue (H&E, ×100). B: High power view of the tumor. Mitotic figures (arrows) are frequently noted (H&E, ×400). C: Tumor cells are positive for c-kit (c-kit immunostain, ×400).
DISCUSSION
This case illustrates a woman who had skull metastasis of imatinib-resistant GIST, which was treated by surgical removal. She lived for one year after craniectomy without evidence of cranial recurrence, and her cause of death was not disease progression itself but infection and respiratory failure.
Although malignant GISTs can theoretically metastasize any organ, they obviously have some tropism for specific organs. They tend to stay in the abdominal cavity even in very advanced stage13). Only a few papers have reported bone metastases of GIST1,5,6,8,10), and the most frequent site of bone metastases re ported were spine and pelvis5,6). Skull metastasis is even rarer. To the best of our knowledge, only five cases of skull metastasis have been reported2,3,9,11,15). Presenting symptoms depended on the location of metastasis, with skull base or periorbital metastases being more symptomatic2–4,11,15).
Management of metastatic GIST should be customized according to symptom, location of disease, available treatment modalities, and condition of the patient. Our patient underwent debulking craniectomy, because we believed that previous long-term imatinib treatment produced a resistant clone, a huge metastatic mass would soon provoke neurologic symptoms, and en-bloc resection would be possible. Debulking surgery is a viable option even in patients with metastatic GIST, especially when disease status is stable or shows limited progression12). If a resistant clone is removed completely, long term survival could be achieved. Our patient survived 10 years after recurrence. Considering that median overall survival of metastatic or recurrent GIST receiving imatinib treatment is five years and nine-year overall survival rate is 34%14), she lived for a comparatively long period after recurrence. We believe that appropriate metastasectomy (peritoneal, hepatic, and skull metastasis) during the treatment course had an important role in her long-term survival.
Traditionally, bone metastasis of GIST was thought to be very rare; however, long-term survival of our patient enabled the disease to metastasize to an uncommon site. Likewise, with the much prolonged survival of GIST patients by virtue of effective target agents and multidisciplinary approach, medical and surgical oncologists will encounter more and more unusual presentations and complications of this disease. For resistant clones, lo cal treatment such as surgery or radiofrequency ablation has a critical role. Therefore, identification of rare but complicated metastasis is essential for clinicians in order to ensure prompt administration of a precise treatment modality.
CONCLUSION
We present the case of a female with skull metastasis of GIST after a long term treatment with imatinib successfully managed by metastasectomy. Symptomatic skull metastasis from GIST is very rare, and an aggressive multidisciplinary approach including surgery and chemotherapy plays an important role in its management.