INTRODUCTION
A categorized disease of spinal deformities, adolescent idiopathic scoliosis (AIS) takes majority of pediatric spinal deformities. Various impacts of the spinal deformity include progression of the deformity, neurological aggravation, cardiopulmonary and psychosocial problems. Since the department of neurosurgery was established in Republic of Korea, the treatment of spinal deformity has not been discussed enough compared to other spinal disorders. However, neurosurgeons have expanded their interests in complex spinal deformities including pediatric spinal deformity such as congenital and adolescent scoliosis4). By high-level technical ability of the spinal cord handling to preserve neurological function, better synergistic effect could be expected. Nevertheless, thorough understanding of pediatric spinal deformity disorders, biology and biomechanics of bone, and metallurgy is absolutely needed. The purpose of this study was to evaluate radiographic and clinical outcomes of AIS patients treated by a Korean neurosurgeon at a single academic center.
MATERIALS AND METHODS
Patients population and the index surgeon
Ten patients who were treated with AIS at our institution between January 2011 and September 2013 were enrolled. The majority were females (7 patients) with average age of 15.3 vs. 15.8. Mean follow-up period was 18.9 month (4-35 months). The index surgeon had been trained by two senior members of scoliosis research society (SRS). One senior mentor was a neurosurgeon and the other's an orthopedic surgeon. He had an oversea instruction by Lenke9) (SRS past-president) for one year. As a neurosurgeon, he has studied orthopedic surgical discipline for spinal deformity surgery.
Pre-and postoperative evaluation
To keep the humerus from blocking visualization of the spine with adequate balance, 36-inch whole spine plain radiographs were checked with fists on clavicle position2). To protect the kids, any radiographs were taken with gonad shield. Spinal curves pattern were classified by Lenke classification and clinical photo including forward bending view of the all patients were taken before and after surgery to compare their clinical gross feature7). Scolisis Resarch Society (SRS-22r) questionnaire was surveyed regularly (preoperative, postoperative six week, one year, two year and so forth) and pulmonary function was examined to assess forced vital capacity (FVC) and forced expiratory volume in one second (FEV1) before and after surgery (one- and two-year after surgery). Number of fusion levels, amount of curve collection by comparison of standing whole spine plain radiographs, surgical complications, radiologic and clinical outcomes were evaluated at every visit to outpatients clinic.
Operative methods
Under general anesthesia, all patients were flipped to prone position on the Jackson spine table. Intraoperative somatosensory evoked potential and trans-cranial motor evoked potential monitoring were set up. Without an any radiographic guidance, all pedicle screws were inserted by freehand technique for segmental instrumentation3,56,8). After screw placement, various correction maneuvers including translation technique, rod derotation, and direct vertebral rotation were utilized for deformity correction. Then, balance of the shoulders and junctional discs was evaluated by portable whole spine radiographs. Sequentially abundant posterior bone graft was performed using local bone with or without allograft bone chips.
RESULTS
Radiographic results
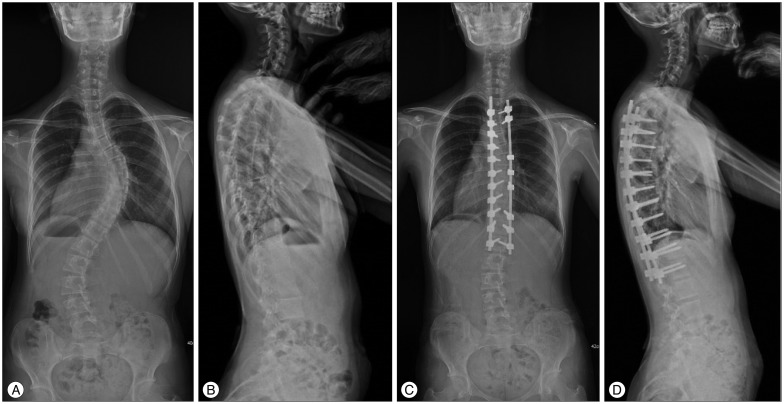
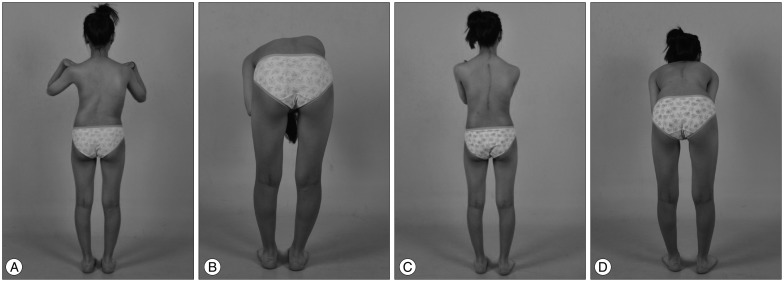
The average number of fusion levels of female and male patients was 10.4 and 12 vertebral bodies, respectively. The range of Cobb angle at structural major curvature was 51-75 degrees. The average percentage of correction of the major structural curve was 73.6% (ranged from 64% to 81.5%) (Fig. 1).
Pulmonary function test
Preoperative and final postoperative absolute FVC averaged 3.03 L and 3.76 L, respectively (0.73 L increase, p=0.046). Preoperative and final postoperative absolute FEV1 averaged 2.63 L and 3.49 L, respectively (0.86 L increase, p=0.021).
Clinical outcomes and complications
Preoperative and final postoperative average self-image and function scores of SRS-22r were, 2.6┬▒0.5, 3.3┬▒0.1, 4.0┬▒0.5, and 4.6┬▒0.0, respectively. Based on the data, significant improvement of the self-image and function scores of SRS-22r questionnaires were achieved through surgery (p<0.05) (Fig. 2). No cases of neurological deficit, infection or screw malposition arose. One patient, however, underwent a revision fusion extension surgery for shoulder asymmetry.
DISCUSSION
Adolescent idiopathic scoliosis typically develops in females around the time of menarche and presents with a conspicuous back or chest-wall deformity. Cosmetic purposes are the most common motivators behind surgery, nevertheless neurological function is normal and symptoms are minimal. Traditionally, orthopedic surgeons have played an important role in the treatment of AIS. This might be attributable to the orthopedic surgeons' experience with osseous fixation for long-bone and skeletal fractures. However, neurosurgeons have recognized that a fundamental understanding of spinal deformity is essential for neurological surgery. For sure, there were several anecdotal cases of AIS diagnosis and treatment by Korean neurosurgeons4,10). Since Korean Spinal Deformity Society has taught Korean neurosurgeons fundamental knowledge of spinal deformity, AIS patients treated by neurosurgeons have increased rapidly.
Classification from King and Moe to Lenke
Adolescent idiopathic scoliosis is first classified by King and Moe at 1983 based on the experience with Harrington rod instrumentation18). To simplify the curve patterns, curves were divided into five types. But, as segmental instrumentation systems began to gain favor by spine surgeons, new classification system which was presented by Lenke in 20019). Lenke classification achieved popularity because of its higher inter- and intra-reliability compared to the King and Moe classification. Although the Lenke classification is more comprehensive and reliable than the King classification, there are still several rule breakers such as 'C' lumbar modifier11).
Surgical indication and timing
A general indication of AIS corrective surgery is as follows : scoliosis exceeding 40┬░ or continued and documented progression of the curvature refractory to brace therapy17). However, health insurance review and assessment service of Republic of Korea permits 15-year-old and older patients having over 50┬░ curvature to undergo corrective surgery. That is the reason why the range of Cobb angle at structural major curvature was 51-75┬░ in this study. Curvature measuring greater than 70┬░ is likely to be associated with cardiopulmonary or neurological symptoms, even after skeletal maturity, making these deficits are more difficult to correct in advanced stages of disease1,1618). In cases of mild scoliosis, brace therapy can be used to delay or even prevent the need for surgery. Often times, surgery is delayed until maximum possible skeletal maturity has occurred. Skeletal maturity is determined by plain radiograph appearance of the iliac apophysis, commonly known as the Risser sign, usually reached at age 14 years in females and age 18 years in males13,1718).
Selection of the level to fuse
If surgical treatment is decided, radiographic analysis is essential to confirm the upper instrumented vertebra (UIV) and lowest instrumented vertebra (LIV). Standing posteroanterior whole spine radiograph including the cervical spine and both hip joints is mandatory. Side bending view is helpful to determine whether a curve is structural or non-structural. After identifying the curve type by Lenke classification9) (curve pattern 1-6 according to major or minor curves, lumbar modifier A-C, sagittal profile hypo-/normo-/hyper-kyphosis), translation and rotation of the apical vertebra is assessed. General rule for selecting the level to fuse is to include the major curve and any structural minor curves. Regarding the approach, anteriorly versus posteriorly, and the actual UIV and LIV are selected by shoulder position and curve type12).
Peri-operative complications and managements
The SRS has been collecting mortality and morbidity database from its members since its foundation in 1965 to assess the complications and adverse outcomes of surgical treatment for spinal deformity. By SRS database, complications were reported in 5.7% of the 6334 patients 14,15). The complications include deep wound infection, pseudarthrosis, neurologic problem, blindness and death. The incidence of surgical complications is not too high, patient and family members expected excellent surgical results because AIS is rarely symptomatic. Peri-operative management is not different with adult spinal deformity, however, external orthosis is not necessarily used owing to good bone quality and modern fixation system.
SRS-22r instrument
After surgery, comparing the results between pre-and postoperative condition is also important. SRS-22r questionnaire results and cardio-pulmonary function tests can be used to evaluate the effectiveness of treatment in terms of functional symptoms, pain, self-image improvement and satisfaction with the operative management. As an evaluation tool for patient's outcome, SRS-questionnaire instrument has been revised from SRS-24 to SRS-22. Nowadays, SRS-22r is widely used. The function, pain, self-image, and mental health domains consisted of five questions and the satisfaction with management domain consisted of two2,14).
Traditionally, orthopedic surgeons are the primary providers of treatment for spinal deformity. Their work has provided major contributions to understanding the biomechanical factors behind spinal correction. However, by treating a subset of spinal deformity patients, neurosurgeons have been making parallel advances in the understanding of spinal disorders6). Regardless of small population, this study shows that the AIS surgery can be performed by a Korean neurosurgeon with acceptable outcomes. However, a fundamental understanding of pediatric spinal deformity and growing spine is essential for the practice of AIS surgery. We recommend any neurosurgeons who want to treat AIS to undergo their training for better knowledge and enhance their surgical skills through our 'Korean Spinal Deformity Society'.