Cho, Shin, Park, and Ji: Efficacy of a Novel Annular Closure Device after Lumbar Discectomy in Korean Patients : A 24-Month Follow-Up of a Randomized Controlled Trial
Abstract
Objective
Lumbar discectomy is an effective treatment for lumbar disc herniation (LDH); however, up to 2-18% of patients with LDH have experienced recurrent disc herniation. The purpose of this study was to evaluate the efficacy of a novel annular closure device (ACD) for preventing LDH recurrence and re-operation compared with that of conventional lumbar discectomy (CLD).
Methods
In this prospective randomized controlled trial, we compared CLD with discectomy utilizing the BarricaidВ® (Intrinsic Therapeutics, Inc., Woburn, MA, USA) ACD. Primary radiologic outcomes included disc height, percentage of preoperative disc height maintained, and re-herniation rates. Additional clinical outcomes included visual analog scale (VAS) scores for back and leg pain, Oswestry Disability Index (ODI) scores, and 12-item short-form health survey (SF-12) quality of life scores. Outcomes were measured at preoperation and at 1 week, 1, 3, 6, 12, and 24 months postoperation.
Results
Sixty patients (30 CLD, 30 ACD) were enrolled in this study. At 24-month follow-up, the disc height in the ACD group was significantly greater than that in the CLD group (11.4Вұ1.5 vs. 10.2Вұ1.2 mm, p=0.006). Re-herniation occurred in one patient in the ACD group versus six patients in the CLD group (ПҮ2=4.04, p=0.044). Back and leg VAS scores, ODI scores, and SF-12 scores improved significantly in both groups compared with preoperative scores in the first 7 days following surgery and remained at significantly improved levels at a 24-month follow-up. However, no statistical difference was found between the two groups.
Conclusion
Lumbar discectomy with the BarricaidВ® (Intrinsic Therapeutics, Inc.) ACD is more effective at maintaining disc height and preventing re-herniation compared with conventional discectomy. Our results suggest that adoption of ACD in lumbar discectomy can help improve the treatment outcome.
Key Words: Intervertebral disc disease В· Discectomy В· Herniated disc В· Barricaid.
INTRODUCTION
Lumbar discectomy is a common surgical procedure performed to relieve symptoms of lumbar disc herniation (LDH), particularly in patients unresponsive to conservative treatment [ 5, 6]. Discectomy addresses radicular symptoms by removing the extruded disc material, thus relieving the symptoms associated with nerve root compression. However, a substantial proportion of the patient population is left with persistent symptoms following discectomy. Discectomy patients reported a postoperative dissatisfaction of 10% to 30% [ 3, 4] and require additional treatment. In general, patients with larger annular defects have higher rates of re-herniation because of the compromised integrity and competence of the annulus. For defects of >6 mm wide, a re-herniation rate of up to 27% has been reported, as opposed to only 4.8% for narrower defects [ 3]. Similarly, patients with defect sizes more than 54 mm2 have reported a re-herniation rate of 18%, which is significantly greater than the 4.7% noted in defects below 36 mm2 [ 13]. Re-operation following discectomy occurs in approximately 20% of cases [ 11], with re-herniation occurring at a rate of 2-18% [ 3, 4, 12, 19] and symptomatic re-herniation of 3-27% [ 4, 5]. A novel annular closure device (ACD) has been developed to improve the outcomes in conventional discectomy. This device has been in clinical use since 2008. It has demonstrated low rates of re-herniation, excellent maintenance of disc height [ 1, 9, 14], and an ability to decelerate facet joint degeneration [ 17]. Previous studies on this device included Caucasian patients. Asians have smaller vertebra and different ratio of cortices [ 8]. Thus, in this study, we aimed to evaluate the efficacy of ACD in improving outcomes following lumbar discectomy compared with that of conventional discectomy in Korean patients.
MATERIALS AND METHODS
Study design and patient selection
All patients were selected from Cham Teun Teun Hospital and Severance Hospital of Yonsei University Medical Center. The Institutional Review Board of Cham Teun Teun Hospital approved the study (IRB approved No. GTIRB-13-005). All patients signed an approved informed consent, and the study was registered publicly prior to enrollment. In this prospective randomized controlled study, a total of 60 patients who were suffering from sciatica unresponsive to conservative treatment of at least 6 weeks duration were included. Patients who met inclusion criteria were selected and asked to consider participating in this clinical trial. Then, patients who agreed to participate in the trial were assigned to the ACD group or the conventional lumbar discectomy (CLD) group using computer-generated randomization codes with a block size of five. To ensure the concealment of intervention assignment, an opaque, sealed envelope that contained randomization codes was opened 1 day prior to the surgery by a blinded clinical research assistant. LDH was confirmed by the presence of localized radicular symptoms and radiographic confirmation via computer tomography and/or magnetic resonance imaging. Patients were randomly divided into two groups of 30 and underwent posterior lumbar discectomy, as follows. In the ACD group, a limited discectomy was followed by implantation of the ACD. In the CLD group, patients underwent CLD alone.
Patient inclusion and exclusion criteria were adopted following previously published protocols [ 10, 14, 17]. Patients were eligible for inclusion if they presented with persistent sciatica with radiographically confirmed herniation and were aged 18 to 75 years. No limitations were placed on the defect height, width, or area, except as defined by the manufacturerвҖҷs instructions for use. Patients were excluded if they met any of the following characteristics : previous back operation, foraminal or extraforaminal disc herniation, extraspinal cause of sciatica, pre-existing spinal pathology, bone mineral density T-score less than -2.0 (for subjects requiring dual-energy X-ray absorptiometry), scoliosis greater than 10 degrees, and other abnormalities, such as spondylolysis and spondylolisthesis, that would potentially interfere with the surgical procedure.
ACD
The Barricaid В® endoprosthesis (Intrinsic Therapeutics, Inc., Woburn, MA, USA) is an implantable ACD designed for use as an adjunct to lumbar discectomy. It functions by blocking the annular defect and maintaining the nucleus pulposus within the anatomic confinement of the disc space. The device consists of two components : a rigid titanium bone anchor ensuring proper fixation on the selected adjacent vertebral body, and a flexible polymer mesh that blocks the defect and prevents further migration of disc material ( Fig. 1). The mesh contains a radiopaque platinum-iridium marker that is embedded in the anchor and allows for radiological identification during implantation. The device has different mesh widths to accommodate varying defect widths.
Surgical techniques
Discectomies were performed under a standard surgical procedure by the same senior neurosurgeon [ 15]. Prophylactic antibiotics were administered upon initiation of the surgical procedure. A medial incision was made for unilateral approach to the interlaminar space. In patients randomized to the ACD group, the ACD was inserted under fluoroscopic control after discectomy ( Fig. 2). In the CLD group, conventional discectomy was performed per standard surgical approach. Following discectomy, the volume of the removed disc material was dry measured and recorded. Procedural duration was recorded for all participants. After surgery, patients were discharged with postoperative instructions according to the surgeonвҖҷs discectomy protocol. No additional bracing or other activity instructions were given to any patient.
Outcome assessment
Patients were assessed postoperatively at 1 week and 1, 3, 6, 12, and 24 months. Primary outcomes included disc height, calculated as the average of the anterior and posterior disc heights, measured on standing lateral radiographs. Postoperative disc height was expressed as both a raw value and as a percentage of the preoperative height. Additional outcomes included patient-reported pain, measured using the visual analog scale (VAS), ranging from 0 to 100. Back and leg pain were recorded separately. Disability was assessed with the Oswestry Disability Index (ODI), which uses scores ranging from 0 to 100 to reflect the degree of disability in patients with low back pain, where higher scores represent more severe disability [ 16]. Health-related quality of life was assessed using the Medical Outcomes Study 12-item short-form health survey (SF-12) scale, which is composed of mental and physical components, where a higher score represents a better quality of life [ 2]. Complications including re-herniation were recorded at follow-up where appropriate. Re-herniation is defined as newly occurred the same side radiculopathy at least 3-point leg VAS and a herniation on the same disc space and on the same side of a previously operated disc level in magnetic resonance imaging (MRI) during follow up period. MRI was performed only in patients with suspected re-herniation to confirm a recurrence.
Statistical analysis
For all quantitative data, descriptive statistics were calculated and recorded as mean and standard deviation. Between-group comparisons for numerical variables were made with the unpaired t-test assuming unequal variances and for categorical variables using the two-tailed chi-square test. Statistical significance was set a priori at p <0.05.
RESULTS
Descriptive statistics
Descriptive statistics are summarized in Table 1. A total of 60 patients were enrolled in the study : 30 in the ACD group and 30 in the CLD group. Nineteen patients were lost to follow-up. At 24 months, data were available for 20 patients in the ACD group and 21 in the CLD group ( Fig. 3). No significant differences were noted in demographic comparisons, including age, sex ratio, body mass index, preoperative symptom duration, disc level, and herniation classification, between the two groups. No significant differences were also noted in preoperative disc height ( Table 1) and preoperative clinical scores, such as VAS for back pain and leg pain, ODI scores, and short form SF-12, between both groups ( Table 2).
Surgical procedure
In all 30 patients in the ACD group, the ACD was implanted at the caudal endplate. An 8-mm implant was used in 83% (25/30) of the patients, and a 10-mm implant in the remaining 17% (5/30). The mean surgical time in the ACD group was significantly longer than that in the control group (143.33Вұ21.43 vs. 126.17Вұ23.37 minutes, p =0.004) ( Table 1). The volume of the removed disc material was significantly less in the ACD group compared with the CLD group (0.5Вұ0.3 vs. 0.9Вұ0.6 mL; p =0.009).
Disc height
No significant difference was found in disc height between the two groups preoperatively (ACD : 13.3Вұ1.2 vs. CLD : 12.9Вұ1.7 mm, p=0.297) ( Table 3). The disc height in the ACD group was maintained and was significantly greater than that in the CLD group in the first 7 days following surgery (ACD : 13.6Вұ1.2 vs. CLD : 11.8Вұ1.7, p=0.01). At 24 months, the disc height in both groups decreased significantly compared with the preoperative disc height (ACD : 11.4Вұ1.5 vs. 13.3Вұ1.2 mm, p <0.001; CLD : 10.2Вұ1.2 vs. 12.9Вұ1.7 mm, p<0.001), with taller disc height in the ACD group than in the CLD group (11.4Вұ1.5 vs. 10.2Вұ1.2 mm, p=0.006) ( Table 3). When evaluated as a percentage of preoperative measures, the disc height was maintained to a significantly greater extent in the ACD group than in the CLD group (86.3Вұ11.5% vs. 79.2Вұ10.0%, p =0.04) ( Table 4).
Patient-related outcomes
At the preoperative period, no significant differences were found in VAS scores for back or leg pain, disability index, and physical and mental SF-12 scores ( Table 2) between the ACD and CLD groups. Comparisons of preoperative and postoperative (24 months) clinical outcomes are listed in Table 5. VAS back scores significantly improved at one week after surgery compared to before surgery (ACD : 62Вұ29 vs. 18Вұ14, p<0.001; CLD : 66Вұ29 vs. 26Вұ17, p<0.001) and remained improved at 24 months (ACD : 20Вұ18, p<0.001 vs. preoperative; CLD : 16Вұ18, p<0.001 vs. preoperative). No significant difference was noted in the changes at preoperation and 24-month follow-up between the groups (29Вұ32 vs. 47Вұ31, p =0.08) ( Fig. 4A). Leg pain improved, with significant improvements noted at 7-day follow-up (ACD : 70Вұ13 vs. 19Вұ18, p <0.001; CLD : 63Вұ26 vs. 25Вұ24, p <0.001), and the improvement remained at 24-month follow-up (ACD : 16Вұ20, p <0.001 vs. preoperative; CLD : 12Вұ18, p<0.001 vs. preoperative). No significant difference was found in leg pain scores between the two groups at 24-month follow-up (ACD : 16Вұ20 vs. CLD : 12Вұ18, p =0.55) ( Fig. 4B). ODI scores were significantly improved at 24-month follow-up versus at preoperation in both the ACD (10Вұ11 vs. 47Вұ15, p <0.001) and CLD (5Вұ5 vs. 52Вұ24, p <0.001) groups. At 24 months, no significant difference was found in ODI scores between the ACD and CLD groups (10Вұ11 vs. 5Вұ5, p =0.08) ( Fig. 5). SF-12 scores significantly improved at 24-month follow-up in both physical (ACD : 26Вұ5, p<0.001 vs. preoperative; CLD : 27Вұ4, p <0.001 vs. preoperative) and mental (ACD : 30Вұ5, p <0.001 vs. preoperative; CLD : 31Вұ5, p <0.001 vs. preoperative) scores in both the ACD and CLD groups. No significant difference was found in either physical (26Вұ5 vs. 27Вұ4, p =0.37) or mental (30Вұ5 vs. 31Вұ5, p =0.40) scores ( Fig. 6) between the two groups at 24-month follow-up.
Disc re-herniation
At 24-month follow-up, re-herniation was reported in one patient in the ACD group, and six cases in the CLD group (ПҮ 2=4.04, p =0.044) ( Fig. 7). No complications, such as device migration, subsidence, loosening, and fracture, were noted in any patient at 24-month follow-up.
DISCUSSION
In the present study, we found that ACD is an effective treatment for back and leg pain caused by single-level LDH, regardless of the LDH type.
Lumbar discectomy is a common procedure used to address LDH. Despite successful lumbar discectomy, symptoms persist in a substantial proportion of patients [ 3, 4]. Re-herniation and re-operation rates above 12% have been reported [ 7], particularly in patients who undergo conservative discectomy, which leaves much of the nucleus intact. The subsequent risk of re-herniation in this group of patients is a concern and leaves many patients susceptible to re-operation [ 11]. Therefore, a novel ACD that allows preservation of much of the nucleus while closing the annular defect has been developed. In this randomized controlled trial, we compared this device to traditional lumbar discectomy. We found that the device preserved lumbar disc height and was associated with significant improvements in pain severity and disability. Our study found that the use of the ACD was successful in helping to maintain the integrity and stability of the annulus, which correlates well with studies examining similar techniques [ 1, 9, 10, 14, 17]. Patients treated with the closure device maintained disc height, when evaluated as both a raw measurement and a percentage of the initial disc height. Our observations that disc height was maintained at 92% and 86% of the initial values at 12 and 24 months, respectively, compares well with other studies that investigated the use of the same ACD described herein. Lequin et al. [ 10] noted a 92.8% maintenance of disc height at a 12-month postoperation and Ledic et al. [ 9] found 91.5% and 90% disc heights at 12- and 24-month follow-ups, respectively. The preservation of disc height in our study was also associated with lower rates of re-herniation when compared with traditional discectomy. Our observation of 3.3% re-herniation rate also corroborates previous studies of this closure device that have demonstrated re-herniation rates of up to 2.9% [ 1, 9, 10, 14], a significant improvement on the rates reported for traditional discectomy, which can reach as high as 20% [ 18]. Finally, our study demonstrated that the device limits the volume of disc material removed when compared with traditional discectomy. By decreasing the volume of resected disc material by 44%, the ACD provides surgeons with the opportunity to perform a less aggressive discectomy. Our findings mirror those of Lequin et al. [ 10], who noted a 20% decrease in the amount of disc material removed with the closure device. Our study reported a mean surgical time of 143 minutes in the ACD group, which was longer than that in the CLD group. This finding is in contrast to other studies of the device, which noted an average surgical time of 120 minutes, a duration not significantly different from the 126 minutes commonly reported for conventional discectomy [ 10]. We hypothesize that this discrepancy could be attributed to inconsistencies in time measurement and recording among the studies, or potentially due to the learning curve associated with the use of the device. Future studies should utilize standardized procedural time measurement techniques and should be performed following the natural learning curve associated with the new technology. As surgeon familiarity with the device increases, the procedural time would naturally decrease. Pain severity and disability scores improved in both the ACD and CLD groups, with both groups demonstrating immediate improvements that were maintained at 24-month follow-up. The improvements in the ACD group, which decreased from preoperative VAS scores of 62 (back) and 70 (leg) to 20 and 16, respectively, at 24 months compare favorably with previous studies that observed decreases in VAS to 15-25/100 at 12 months and 10-20/100 at 24 months [ 9, 10]. Similarly, ODI scores improved from 47 at preoperation to 10 at 24-month follow-up, mirroring other studies that found ODI decreased to 15/100 at both 12 and 24 months post-surgery [ 9, 10]. This study has two important limitations. First, the 2-year follow-up, in which 70% or fewer patients were actually followed up, was short and limited the veracity with which conclusions can be applied in the long term. However, it provided important early information regarding the stability and survivability of the device. Our observations mirror those of other researchers who investigated this ACD and found that the device ensures maintenance of favorable clinical scores and lower rates of re-herniation. Second, the low sample size of our cohort limited the ability to extrapolate results to larger populations. Despite this limitation, the randomized nature of the study provided the highest level of evidence available, and the use of a control group comprised of patients undergoing conventional discectomy provided a valid and important comparison.
CONCLUSIONS
Our findings indicated that the BarricaidВ® (Intrinsic Therapeutics, Inc.) ACD is associated with excellent clinical scores following lumbar discectomy. A superior ability to maintain disc height and decrease re-herniation rates when compared with CLD in Korean patients was also demonstrated. When combined with the existing literature on ACD, these results provide a strong evidence to support its adoption to improve lumbar discectomy outcomes.
Acknowledgements
This work was supported by the Industrial R&D program of MOTIE/KEIT (10043086).
Fig.В 1.
The BarricaidВ® (Intrinsic Therapeutics, Inc., Woburn, MA, USA) implant design. This is formed from a flexible mesh comprising multiple layers of counter-angulated fibers and a strong titanium bone anchor (A). Position of implant in intervertebral space (B). 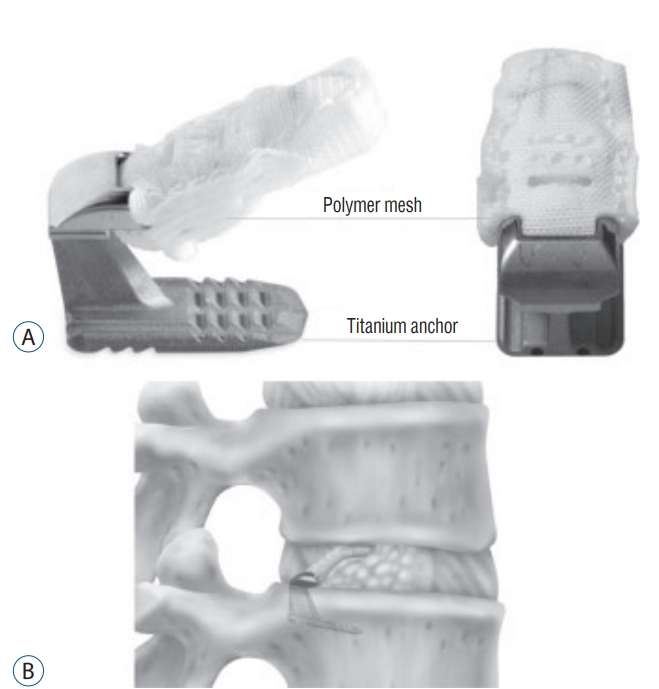
Fig.В 2.
BarricaidВ® (Intrinsic Therapeutics, Inc., Woburn, MA, USA) endoprosthesis implanted in targeted disc space. A : Schematic representation of device by means of specialized delivery tool. Arrow : fixed the Barricaid to the upper vertebral body using a specialized delivery tool. B : X-ray image of positioned device in L4/5 intervertebral space. 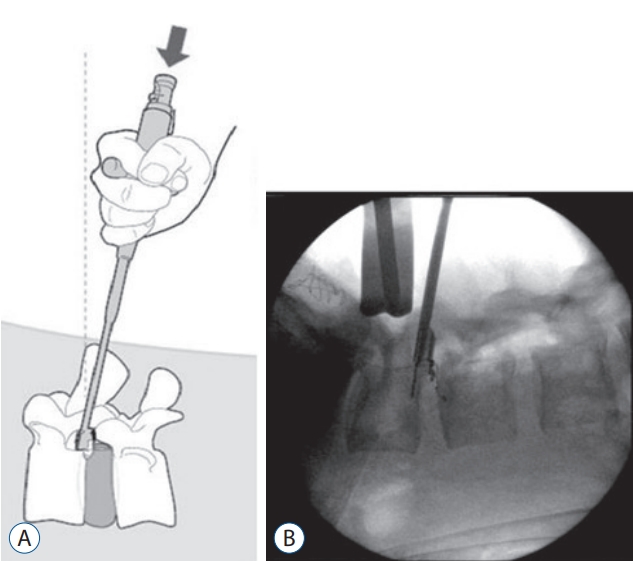
Fig.В 3.
Number of follow-up patients from preoperative to 24-month follow-up. ACD : annular closure device, CLD : conventional lumbar discectomy. 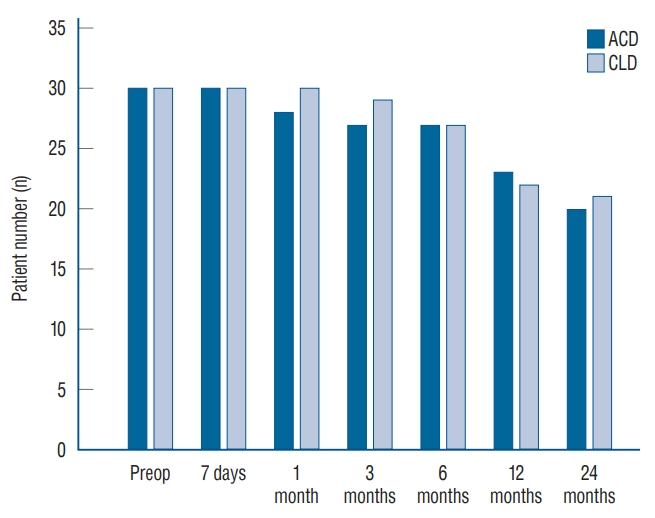
Fig.В 4.
VAS back (A) and leg (B) pain scores from preoperative to 24-month follow-up. ACD : annular closure device, CLD : conventional lumbar discectomy. 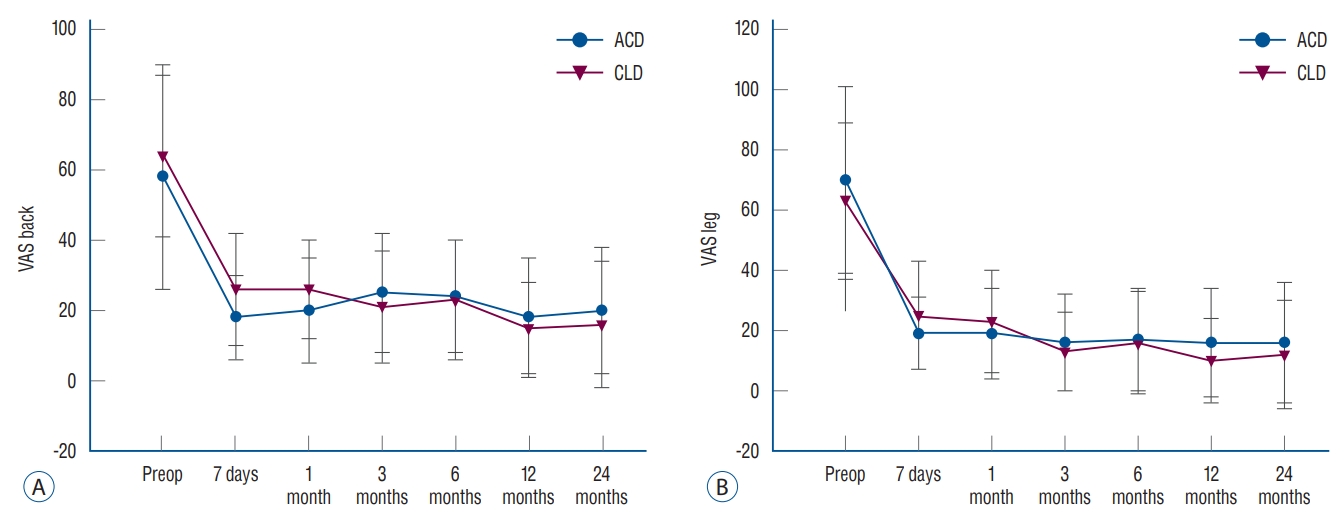
Fig.В 5.
Oswestry Disability Index (ODI) scores from preoperative to 24-month follow-up. ACD : annular closure device, CLD : conventional lumbar discectomy. 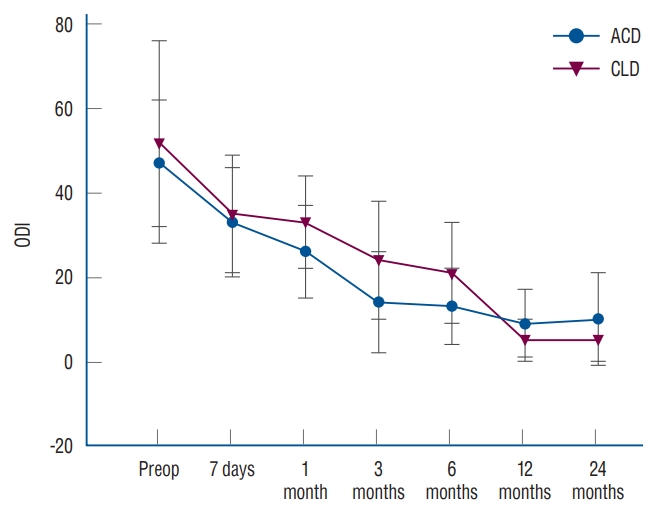
Fig.В 6.
Quality of life, physical (SF-12 PCS : A) and mental (SF-12 MCS : B) scores from preoperative to 24-month follow-up. ACD : annular closure device, CLD : conventional lumbar discectomy, SF-12 : 12-item short-form health survey scale, PCS : physical component summary, MCS : mental component summary. 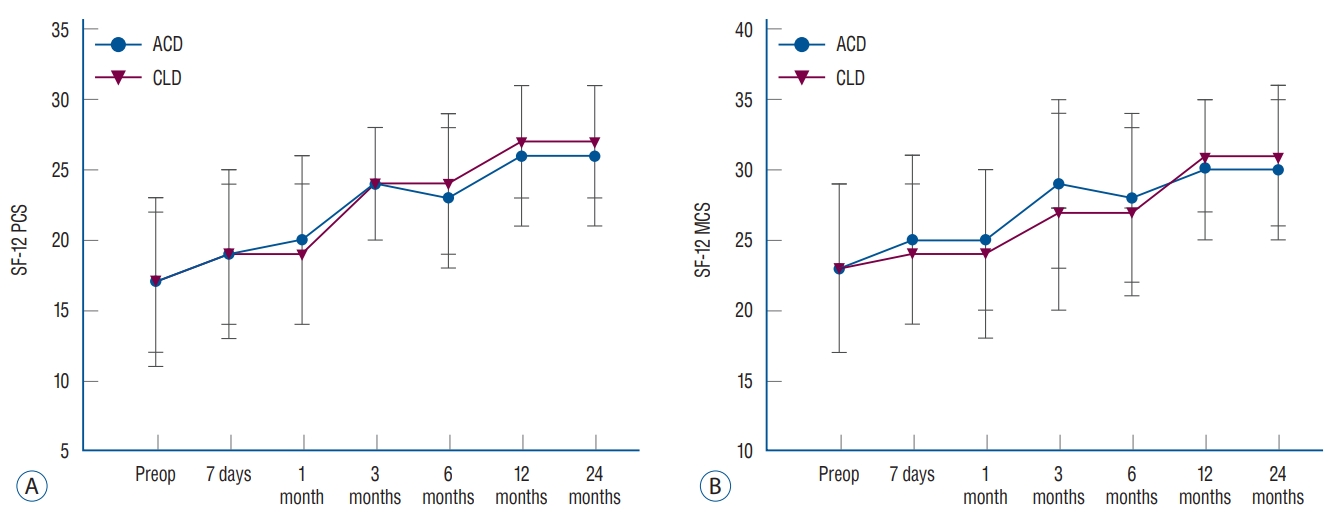
Fig.В 7.
Disc recurrence at 24-months after surgery. *p<0.005. ACD : annular closure device, CLD : conventional lumbar discectomy. 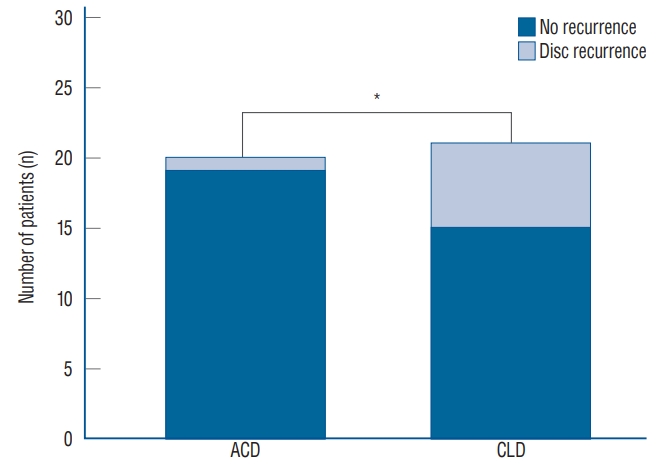
TableВ 1.
Demographics and characteristics in ACD and CLD group
|
ACD |
CLD |
p-value |
|
Number |
30 |
30 |
|
|
Age (years) |
41.37Вұ10.86 |
42.63Вұ11.51 |
0.663 |
|
Sex (M : F) |
20 : 10 |
25 : 5 |
0.136 |
|
BMI |
24.41Вұ3.40 |
24.43Вұ3.23 |
0.984 |
|
Symptom duration (weeks) |
22.13Вұ15.81 |
33.30Вұ48.59 |
0.236 |
|
Operation level |
|
|
0.374 |
|
вҖғL3-L4 |
1 |
4 |
|
|
вҖғL4-L5 |
17 |
15 (or 13*) |
|
|
вҖғL5-S1 |
12 |
11 (or 13*) |
|
|
Herniation classification |
|
|
0.078 |
|
вҖғProtrusion |
5 |
3 |
|
|
вҖғExtrusion |
16 |
24 |
|
|
вҖғSequestration |
9 |
3 |
|
|
Operation time (minutes) |
143.33Вұ21.43 |
126.17Вұ23.37 |
0.004 |
|
Preoperative disc height (mm) |
13.3Вұ1.2 |
12.9Вұ1.7 |
0.297 |
|
Volume of removed disc (mL) |
0.5Вұ0.3 |
0.9Вұ0.6 |
0.009 |
TableВ 2.
Preoperative clinical outcomes of VAS, ODI, and SF-12
|
Outcome |
ACD |
CLD |
p-value |
|
VAS back pain |
58Вұ32 |
64Вұ23 |
0.408 |
|
VAS leg pain |
70Вұ31 |
63Вұ26 |
0.348 |
|
SF-12 P |
17Вұ5 |
17Вұ6 |
0.853 |
|
SF-12 M |
23Вұ6 |
23Вұ6 |
1.000 |
|
ODI |
47Вұ15 |
52Вұ24 |
0.361 |
TableВ 3.
Disc height changes from preoperative to 24-month follow-up
|
ACD (mm) |
CLD (mm) |
p-value |
|
Preoperative |
13.3Вұ1.2 |
12.9Вұ1.7 |
0.297 |
|
Postoperative |
|
|
|
|
вҖғ7 days |
13.6Вұ1.2 |
11.8Вұ1.7 |
0.001 |
|
вҖғ1 month |
13.4Вұ1.2 |
12.1Вұ1.9 |
0.003 |
|
вҖғ3 months |
12.7Вұ1.3 |
11.2Вұ1.6 |
0.001 |
|
вҖғ6 months |
12.2Вұ1.4 |
10.9Вұ1.6 |
0.001 |
|
вҖғ12 months |
12.0Вұ1.3 |
10.8Вұ1.2 |
0.007 |
|
вҖғ24 months |
11.4Вұ1.5*
|
10.2Вұ1.2*
|
0.007 |
TableВ 4.
Mean percentage of preoperative disc height at each time point from 7-day to 24-month follow-up
|
ACD (%) |
CLD (%) |
p-value |
|
Postoperative |
|
|
|
|
вҖғ7 days |
102.4Вұ4.8 |
92.0Вұ7.6 |
<0.001 |
|
вҖғ1 month |
100.8Вұ5.6 |
93.9Вұ8.3 |
<0.001 |
|
вҖғ3 months |
96.5Вұ9.2 |
86.9Вұ8.4 |
<0.001 |
|
вҖғ6 months |
92.1Вұ10.2 |
83.7Вұ9.2 |
0.002 |
|
вҖғ12 months |
91.8Вұ10.2 |
84.2Вұ9.0 |
0.014 |
|
вҖғ24 months |
86.3Вұ11 |
79.2Вұ10.0 |
0.044 |
TableВ 5.
Comparison of clinical outcomes between preoperative and 24-month
|
Outcome |
ACD
|
CLD
|
|
Preop |
Postop 24-month |
Preop |
Postop 24-month |
|
VAS back pain |
62Вұ29 |
20Вұ18 |
66Вұ20 |
16Вұ18 |
|
VAS leg pain |
70Вұ31 |
16Вұ20 |
63Вұ26 |
12Вұ18 |
|
SF-12 P |
17Вұ5 |
26Вұ5 |
17Вұ6 |
27Вұ4 |
|
SF-12 M |
23Вұ6 |
30Вұ5 |
23Вұ6 |
31Вұ5 |
|
ODI |
47Вұ15 |
10Вұ11 |
52Вұ24 |
5Вұ5 |
References
2. Brazier JE, Harper R, Jones NM, OвҖҷCathain A, Thomas KJ, Usherwood T, et al : Validating the SF-36 health survey questionnaire: new outcome measure for primary care. BMJ 305 : 160-164, 1992    3. Carragee EJ, Han MY, Suen PW, Kim D : Clinical outcomes after lumbar discectomy for sciatica: the effects of fragment type and anular competence. J Bone Joint Surg Am 85 : 102-108, 2003   4. Carragee EJ, Spinnickie AO, Alamin TF, Paragioudakis S : A prospective controlled study of limited versus subtotal posterior discectomy: shortterm outcomes in patients with herniated lumbar intervertebral discs and large posterior anular defect. Spine (Phila Pa 1976) 31 : 653-657, 2006   5. Davis RA : A long-term outcome analysis of 984 surgically treated herniated lumbar discs. J Neurosurg 80 : 415-421, 1994   6. Gray DT, Deyo RA, Kreuter W, Mirza SK, Heagerty PJ, Comstock BA, et al : Population-based trends in volumes and rates of ambulatory lumbar spine surgery. Spine (Phila Pa 1976) 31 : 1957-1963, 2006   7. Heindel P, Tuchman A, Hsieh PC, Pham MH, DвҖҷOro A, Patel NN, et al : Reoperation rates after single-level lumbar discectomy. Spine (Phila Pa 1976) 42 : E496-E501, 2017   8. Kepley AL, Nishiyama KK, Zhou B, Wang J, Zhang C, McMahon DJ, et al : Differences in bone quality and strength between Asian and Caucasian young men. Osteoporos Int 28 : 549-558, 2017    9. Ledic D, Vukas D, Grahovac G, Barth M, Bouma GJ, Vilendecic M : Effect of anular closure on disk height maintenance and reoperated recurrent herniation following lumbar diskectomy: two-year data. J Neurol Surg A Cent Eur Neurosurg 76 : 211-218, 2015    11. Martin BI, Mirza SK, Flum DR, Wickizer TM, Heagerty PJ, Lenkoski AF, et al : Repeat surgery after lumbar decompression for herniated disc: the quality implications of hospital and surgeon variation. Spine J 12 : 89-97, 2012   12. McGirt MJ, Ambrossi GL, Datoo G, Sciubba DM, Witham TF, Wolinsky JP, et al : Recurrent disc herniation and long-term back pain after primary lumbar discectomy: review of outcomes reported for limited versus aggressive disc removal. Neurosurgery 64 : 338-344, 2009   13. McGirt MJ, Eustacchio S, Varga P, Vilendecic M, Trummer M, Gorensek M, et al : A prospective cohort study of close interval computed tomography and magnetic resonance imaging after primary lumbar discectomy: factors associated with recurrent disc herniation and disc height loss. Spine (Phila Pa 1976) 34 : 2044-2051, 2009   14. Parker SL, Grahovac G, Vukas D, Vilendecic M, Ledic D, McGirt MJ, et al : Effect of an annular closure device (barricaid) on same-level recurrent disk herniation and disk height loss after primary lumbar discectomy: two-year results of a multicenter prospective cohort study. Clin Spine Surg 10 : 454-460, 2016  15. Spengler DM : Lumbar discectomy. Results with limited disc excision and selective foraminotomy. Spine (Phila Pa 1976) 7 : 604-607, 1982   16. StrГ¶mqvist B, Fritzell P, HГӨgg O, JГ¶nsson B, Swedish Society of Spinal Surgeons : The Swedish spine register: development, design and utility. Eur Spine J 18 Suppl 3 : 294-304, 2009   17. Trummer M, Eustacchio S, Barth M, Klassen PD, Stein S : Protecting facet joints post-lumbar discectomy: barricaid annular closure device reduces risk of facet degeneration. Clin Neurol Neurosurg 115 : 1440-1445, 2013   18. Watters WC 3rd, McGirt MJ : An evidence-based review of the literature on the consequences of conservative versus aggressive discectomy for the treatment of primary disc herniation with radiculopathy. Spine J 9 : 240-257, 2009   19. Yorimitsu E, Chiba K, Toyama Y, Hirabayashi K : Long-term outcomes of standard discectomy for lumbar disc herniation: a follow-up study of more than 10 years. Spine (Phila Pa 1976) 26 : 652-657, 2001  
|
|























