Park, Choi, Kim, Kim, and Hong: Modified Graded Repair of Cerebrospinal Fluid Leaks in Endoscopic Endonasal Transsphenoidal Surgery
Abstract
Objective
Complete sellar floor reconstruction is critical to avoid postoperative cerebrospinal fluid (CSF) leakage during transsphenoidal surgery. Recently, the pedicled nasoseptal flap has undergone many modifications and eventually proved to be valuable and efficient. However, using these nasoseptal flaps in all patients who undergo transsphenoidal surgery, including those who had none or only minor CSF leakage, appears to be overly invasive and time-consuming.
Methods
Patients undergoing endoscopic endonasal transsphenoidal tumor surgery within a 5 year-period were reviewed. Since 2009, we classified the intraoperative CSF leakage into grades from 0 to 3. Sellar floor reconstruction was tailored to each leak grade. We did not use any tissue grafts such as abdominal fat and did not include any procedures of CSF diversions such as lumbar drainage.
Results
Among 200 cases in 188 patients (147 pituitary adenoma and 41 other pathologies), intraoperative CSF leakage was observed in 27.4% of 197 cases : 14.7% Grade 1, 4.6% Grade 2a, 3.0% Grade 2b, and 5.1% Grade 3. Postoperative CSF leakage was observed in none of the cases. Septal bone buttress was used for Grade 1 to 3 leakages instead of any other foreign materials. Pedicled nasoseptal flap was used for Grades 2b and 3 leakages. Unused septal bones and nasoseptal flaps were repositioned.
Conclusion
Modified classification of intraoperative CSF leaks and tailored repair technique in a multilayered fashion using an en-bloc harvested septal bone and vascularized nasoseptal flaps is an effective and reliable method for the prevention of postoperative CSF leaks.
Key Words: Cerebrospinal fluid leak · Endoscopy · Skull base · Pituitary adenoma · Complications · Outcome.
INTRODUCTION
Since the introduction of endoscopy for transsphenoidal pituitary surgery in 1992, endoscopic endonasal transsphenoidal approach (EETSA) for sellar and parasellar regions has been considerably advanced 13). EETSA is a minimally invasive technique that is considered to be safe and effective for treatment of pituitary adenoma and other parasellar lesions. However, EETSA allows only for a very limited space for instrument manipulation and results in difficulties in dura repair for cerebrospinal fluid (CSF) leak after tumor removal. If not completely controlled during surgery, postoperative CSF leaks may be troublesome. Long-term bed rest, CSF diversion techniques, and revision surgery for sellar floor reconstruction may be needed for the management of CSF leaks and prevention of related complications, such as meningitis and tension pneumocephalus. Thus, in order to avoid postoperative CSF leaks, it is essential to achieve the complete sellar floor reconstruction. Many different reconstruction materials and methods using autologous and synthetic materials have been introduced 1,811,1416,1822). Moreover, a graded repair approach to CSF leaks after EETSA has been introduced; however, the outcome was insufficient, especially in large diaphragmatic defects 7). Recently, a novel method using a pedicled nasoseptal flap (NSF) was introduced and used for the cases in which large intraoperative CSF leaks occurred by large diaphragmatic defects 9,1017). Thereafter, a modification of NSF elevation method has been reported, in detail, by several surgeons 19,2932,35). This report provides a detailed account of our experience using a modified CSF leak grading and repair protocol. Since 2009, we started performing EETSAs with a modified graded repair technique to prevent CSF leaks. Patients undergoing EETSA within a 5 year-period were reviewed. In this paper, we introduce our reliable and effective method of the modified graded repair technique.
MATERIALS AND METHODS
Approval for this study was granted by the Institutional Review Board of Seoul St. Mary's Hospital. We retrospectively reviewed the patients who underwent EETSA in our institute from January 2009 to December 2013 (i.e., the 5-year period). The total number of patients was 188. Additionally, a total of 200 operations, including recurrent tumors, were performed. Since January of 2009, we classified the intraoperative CSF leakage into grades from 0 to 3 ( Fig. 1). We modified the grading system of CSF leaks initially introduced in 2007 by Esposito et al. 7). The medical records of 188 patients were reviewed and analyzed by the present authors. The operative records, including notes and video, as well as other medical records, were reviewed to identify procedure-related complications. All patients were followed postoperatively for at least 3 months and were monitored with endoscopic examinations and imaging.
Surgical technique
All operations were performed via two nostrils-four hands technique in which the main surgeon freely uses two surgical instruments and an assistant neurosurgeon holds the endoscope using a different instrument. The nasal and sphenoid stage was performed by a rhinology surgeon, the sellar stage was performed by a neurosurgeon, and sellar repair was performed by both surgeons. The patient's head was positioned on a horseshoe head rest and an electromagnetic navigation system (Medtronics®, Louisville, KY, USA) was used for all patients. During the approach, the bilateral inferior turbinates were outfractured and both middle turbinates were fully lateralized. Furthermore, we lateralized the superior turbinate and confirmed the natural orifice of the sphenoid sinus. We used bilateral modified "rescue" flaps introduced by Kim et al. 19). The flap was designed on the right side of the nasal septum. A curvilinear incision was made from the inferior border of the sphenoidal sinus ostium following the sagittal plane of the septum with monopolar sharp electrocautery. This incision was made anteriorly toward the level of one-half to one-third the height of the middle turbinate over the vomer to preserve the nasoseptal pedicle ( Fig. 1A). A mucoperiosteal flap was made from the right side of the bony nasal septum with Cottle and hockey stick elevators ( Fig. 1B). The right ostium of the sphenoidal sinus was widened superiorly and inferiorly with a rongeur. After elevating the right modified nasoseptal rescue flap, the posterior bony septum that included a portion of the perpendicular plate of the ethmoid bone, the vomer, and the anterior wall of the sphenoidal sinus was removed in en-bloc fashion. We attempted to harvest the posterior septal bone in an en-bloc fashion for use in sellar floor reconstruction. The sellar floor was exposed after the procedure and a left-side modified "rescue" flap was made along the border of the removed septal bone. To avoid any injuries affecting the potential use of those flaps, both NSFs were displaced into the nasopharynx. Then, we removed the sphenoid septum and reflected the sphenoid mucosa laterally to cover the sphenoid sinus again during the sellar repair. The sellar floor was drilled out, the dura was opened, and the tumor was removed under the two nostrils-four hands technique by two neurosurgeons (the main surgeon and the assistant). Intraoperative CSF leaks were graded according to the modified CSF leak grading system ( Fig. 2). The repair protocol for each grade is summarized in Fig. 3. In cases of no intraoperative CSF leaks, sellar reconstruction was not performed. In cases of small "weeping" leaks (Grade 1), sellar reconstruction was performed in a multilayered fashion with oxidative cellulose packing (Surgicel®, Ethicon; Johnson & Johnson, Somerville, NJ, USA), outlay dural substitutes (Duraform®, Codman; Johnson & Johnson, Raynham, MA, USA) as the first layer and the placement of prepared septal bone into the bony defect of the sellar floor as the second layer. Furthermore, the reflected sphenoid mucosa was repositioned for coverage of the operation site as the third layer and a tissue sealant (DuraSeal®, Covidien, Dublin, Ireland) was applied as the fourth layer. When too much of the sphenoid mucosa had been removed, the left modified "rescue" flap was used instead of the sphenoid mucosa as the third layer. If there was a moderate CSF leak with an obvious diaphragmatic defect (grade 2a), the diaphragmatic defect site was sealed with a collagen hemostatic agent (TachoComb®, CSL Behring, Tokyo, Japan) and a multilayered technique, as for grade 1 repair, was used. When a CSF leak was observed after septal bone insertion with the Valsalva maneuver (grade 2b), the right conventional flap was applied to the denuded sphenoid sinus as the third layer and tissue sealant was spread over the NSF as the fourth layer. In cases of large CSF leaks (grade 3), sellar repair with an inlay and outlay dural substitutes, septal bone, and a pedicled NSF was performed ( Fig. 3, 4). Pedicled NSFs (conventional NSFs) were made by extending the incision of initial approach, which is decribed previously in term of modified "rescue" flap, only in the cases of grade 2b and grade 3 CSF leaks. The unused NSFs were repositioned to the origin site of the flap and unused posterior septal bone was inserted between the bilateral nasoseptal flaps. Nasal packing was performed with biodegradable fragmentable foam (Nasopore®, Polyganics, Groningen, The Netherlands) and polyvinyl alcohol sponge (Merocel®, Medtronic Xomed Surgical Products, Jacksonville, FL, USA) which was removed on day 3 postoperatively. For patients with grade 1 to 3 CSF leaks, one day of bed rest was sufficient.
RESULTS
Among 200 cases in 188 patients (147 pituitary adenoma and 41 other pathologies), 3 cases (1.5%) were excluded due to preoperative infection. The mean age of the patients was 46.6 years, and there were more female patients (54.4%). Visual disturbance was the most frequent symptom, followed by hormonal symptom. Table 2 outlines the pathologic entities of all patients. The most common pathology was pituitary adenoma. The mean size of tumors was 2.54 cm (range from 0.6 to 9.8 cm). Intraoperative CSF leakage was observed in 27.4% of the 197 cases ( Table 3), specifically : 14.7% grade 1, 4.6% grade 2a, 3.0% grade 2b, and 5.1% grade 3. The sellar floor was reconstructed according to the CSF leak grading system ( Table 1, 4). There were no cases of postoperative CSF leakage. Septal bone buttress was used for Grades 1 to 3 leakages instead of any other foreign materials. Pedicled nasoseptal flap was used for grades 2b and 3 leakages. Especially in grade 3 CSF leaks, in which the outcome of CSF leak repair was not sufficient in other reports 2,57,1215,1826,2932), all cases with applied pedicled NSF had no postoperative CSF leaks and the flaps became mucosalized 6 to 12 weeks after surgery. grade 2b CSF leaks occurred in chordomas (2 cases), craniopharyngiomas (2 cases) and tuberculum sellae meningiomas (2 cases). Moreover, grade 3 CSF leaks occurred in chordomas (5 cases), craniopharyngiomas (4 cases) and pituitary adenoma (1 case). Unused septal bones and nasoseptal flaps were repositioned. Abdominal fat graft or lumbar CSF diversion was completely unnecessary. The common complications after surgery were panhypopituitarism (5.6%) and diabetes insipidus (3.6%) ( Table 5). There were two meningitis cases without postoperative CSF leaks (1.0%) and all patients recovered with an antibiotics therapy. To assess several nasal symptoms, all patients underwent preoperative nasal evaluation using Nasal Obstruction Symptom Evaluation (NOSE), Sino-Nasal Outcome Test (SNOT-20), and a visual analogue scale (VAS), and the repeat tests were performed 6 months postoperatively. There was no significant difference between the preoperative and postoperative NOSE scores and SNOT-20 scores. However, according to a VAS score, nasal symptoms of subjectively decreased olfactory function were observed in the patients with elevated NSFs ( p<0.05) 19,20).
DISCUSSION
Postoperative CSF leak is a serious potential problem following EETSA. While the rate of postoperative CSF leaks after pituitary surgery is lower than 5%, the incidence after extended endoscopic TSA is higher than in the traditional sellar approach 3,46,1721,28). The reliable reconstruction of the sellar floor against intraoperative CSF leaks during EETSA is essential in order to avoid unfavorable postoperative outcomes. To this end, many surgeons have introduced a variety of sellar reconstruction materials and methods. Autologous materials, such as fat, fascia, and muscle graft, and synthetic materials, including alumina ceramic, stainless steel, silicon, titanium, vicryl patches, and collagen fleece, have been recommended and used 1,78,1114,1618,2224,3435,37). While all of the above can be effective for prevention of postoperative CSF leaks, some of these materials have disadvantages. A secondary incision in the abdomen, thigh, or nasal mucosa was needed for harvesting autologous fat, muscle, fascia, septal cartilage, and bone. Similarly, several synthetic materials provoked host-tissue reactions and the distortion of magnetic resonance images 25,34). In this report, we provide a detailed account of our experience using a modified CSF leak grading and repair protocol. Since 2009, we started using the two nostrils-four hands technique to perform EETSA more comfortably. To facilitate this technique, a larger posterior septectomy was needed, because it provided a wider working space and surgical view for the neurosurgeon. However, massive destruction of the bilateral posterior septal mucosa and bone induced nasal morbidity, such as nasal crusting, rhinolalia, and olfactory disturbance 35). Thus, we patientselevated bilateral NSFs and removed posterior septal bone as en-bloc in all EETSA cases and were able to perform two nostrils-four hands technique without massive destruction of posterior septum. In addition, potential sellar floor reconstruction materials including septal bone and pedicled NSF could be obtained in the process of bilateral NSFs elevation. As these materials were used in a multilayered fashion according to the CSF leak grading system, complete sellar floor reconstruction could be achieved without additional incisions in the abdomen, thigh, or nasal mucosa, as well as without postoperative CSF diversion. Esposito et al. 7) introduced multilayered sellar repair methods without nasoseptal flaps according to the CSF leak grading system. Postoperative CSF leak rate was low in grades 0, 1, and 2 CSF leaks (0.7%, 3%, and 1%, respectively), but high (12%) in grade 3 in spite of intrasellar and sphenoid sinus fat packing, onlay titanium mesh, and the insertion of lumbar drainage postoperatively. We used no abdominal fat, fascia lata, or CSF diversion techniques and achieved a good surgical outcome with septal bone buttress and NSFs in grades 2 and 3 CSF leaks. There are several reports where multilayered sellar floor reconstruction was performed with NSFs and where the reported postoperative CSF leak rate ranged from 3.1% to 5.4% in high-flow CSF leaks 17,26). While in these studies a unilateral NSF was elevated in cases of anticipated high-flow CSF leaks, we routinely make bilateral NSFs in EETSA because the flaps are not only for sellar floor reconstruction, but also for two nostrils-four hands technique. We achieved the complete sellar floor reconstruction with bilateral NSFs and septal bone and simultaneously obtained a wide operation field and working space preventing the conflicting interaction of endoscopic instruments. The bilateral NSFs elevation has the advantage of repositioning the unused bone and flaps and allows for dealing with unexpected intraoperative CSF leaks. Repositioning of unused bone and flaps makes it possible to restore the patients' nasal septum postoperatively and minimize the septal defect and nasal morbidity. Moreover, during the revision surgery, we were able to elevate the NSFs again and use the repositioned septal bone and NSFs for sellar floor reconstruction. Preparing NSFs can be essential in the reconstruction of sellar floor with an unexpected intraoperative CSF leak during EETSA. All NSFs were well mucosalized on the sellar floor and there was no postoperative CSF leak.
The nasoseptal flap-related complications were postoperatively decreased olfactory function. VAS scores for olfactory functional disturbance worsened significantly; however, other parameters, including VAS for nasal stuffiness, rhinorrhea, sneezing, and obstruction, showed no significant differences after the surgery. Careful attention and meticulous manipulation of nasal structures is necessary for surgeons not to injure the olfactory neuroepithelium. Further investigations to reduce olfactory dysfunction after EETSA are necessary. Minimizing the incision and surgical approach during the nasal stage could be an alternative option to preserve olfactory function.
CONCLUSION
Patients undergoing EETSA within a 5 year-period were reviewed and the overall postoperative CSF leak rate for those 5 years was 0.0% (0 of 197 cases). To our knowledge, this modified graded repair technique shows the most successful outcome compared to other reports 7,1017,2430,3137). Modified classification of intraoperative CSF leaks and tailored repair technique in a multilayered fashion using an en-bloc harvested septal bone and vascularized nasoseptal flaps is an effective and reliable method for the prevention of postoperative CSF leak. Without using any artificial grafts, abdominal fat graft, and lumbar CSF diversion, this method is considerably more convenient and successful for intraoperative CSF leaks.
References
1. Arita K, Kurisu K, Tominaga A, Ikawa F, Iida K, Hama S, et al : Size-adjustable titanium plate for reconstruction of the sella turcica. Technical note. J Neurosurg 1999, 91 : 1055-1057,   2. Berker M, Hazer DB, Yücel T, Gürlek A, Cila A, Aldur M, et al : Complications of endoscopic surgery of the pituitary adenomas : analysis of 570 patients and review of the literature. Pituitary 2012, 15 : 288-300,   3. Cappabianca P, Cavallo LM, Colao A, de Divitiis E : Surgical complications associated with the endoscopic endonasal transsphenoidal approach for pituitary adenomas. J Neurosurg 2002, 97 : 293-298,   4. Cappabianca P, Cavallo LM, Esposito F, Valente V, De Divitiis E : Sellar repair in endoscopic endonasal transsphenoidal surgery : results of 170 cases. Neurosurgery 2002, 51 : 1365-1371, discussion 1371-1372   5. Cho JM, Ahn JY, Chang JH, Kim SH : Prevention of cerebrospinal fluid rhinorrhea after transsphenoidal surgery by collagen fleece coated with fibrin sealant without autologous tissue graft or postoperative lumbar drainage. Neurosurgery 2011, 68( 1 Suppl Operative):130-136, discussion 136-137   6. Couldwell WT, Weiss MH, Rabb C, Liu JK, Apfelbaum RI, Fukushima T : Variations on the standard transsphenoidal approach to the sellar region, with emphasis on the extended approaches and parasellar approaches : surgical experience in 105 cases. Neurosurgery 2004, 55 : 539-547, discussion 547-550   7. Esposito F, Dusick JR, Fatemi N, Kelly DF : Graded repair of cranial base defects and cerebrospinal fluid leaks in transsphenoidal surgery. Neurosurgery 2007, 60( 4 Suppl 2):295-303, discussion 303-304  8. Freidberg SR, Hybels RL, Bohigian RK : Closure of cerebrospinal fluid leakage after transsphenoidal surgery : technical note. Neurosurgery 1994, 35 : 159-160,   9. Goel A, Muzumdar DP : Reconstruction of the sella floor using vascularized pedicled mucosal flap. Br J Neurosurg 2003, 17 : 553-555,   10. Hadad G, Bassagasteguy L, Carrau RL, Mataza JC, Kassam A, Snyderman CH, et al : A novel reconstructive technique after endoscopic expanded endonasal approaches : vascular pedicle nasoseptal flap. Laryngoscope 2006, 116 : 1882-1886,   11. Hardy J : Transsphenoidal hypophysectomy. J Neurosurg 1971, 34 : 582-594,   12. Horridge M, Jesurasa A, Olubajo F, Mirza S, Sinha S : The use of the nasoseptal flap to reduce the rate of post-operative cerebrospinal fluid leaks following endoscopic trans-sphenoidal surgery for pituitary disease. Br J Neurosurg 2013, 27 : 739-741,   13. Jankowski R, Auque J, Simon C, Marchal JC, Hepner H, Wayoff M : Endoscopic pituitary tumor surgery. Laryngoscope 1992, 102 : 198-202,   14. Kabuto M, Kubota T, Kobayashi H, Takeuchi H, Nakagawa T, Kitai R, et al : Long-term evaluation of reconstruction of the sellar floor with a silicone plate in transsphenoidal surgery. J Neurosurg 1998, 88 : 949-953,   15. Kaptain GJ, Kanter AS, Hamilton DK, Laws ER : Management and implications of intraoperative cerebrospinal fluid leak in transnasoseptal transsphenoidal microsurgery. Neurosurgery 2011, 68( 1 Suppl Operative):144-150, discussion 150-151   16. Kaptain GJ, Vincent DA, Laws ER Jr : Cranial base reconstruction after transsphenoidal surgery with bioabsorbable implants. Neurosurgery 2001, 48 : 232-233, discussion 233-234   17. Kassam AB, Thomas A, Carrau RL, Snyderman CH, Vescan A, Prevedello D, et al : Endoscopic reconstruction of the cranial base using a pedicled nasoseptal flap. Neurosurgery 2008, 63( 1 Suppl 1):ONS44-ONS52, discussion ONS52-ONS53   18. Kelly DF, Oskouian RJ, Fineman I : Collagen sponge repair of small cerebrospinal fluid leaks obviates tissue grafts and cerebrospinal fluid diversion after pituitary surgery. Neurosurgery 2001, 49 : 885-889, discussion 889-890   19. Kim BY, Shin JH, Kang SG, Kim SW, Hong YK, Jeun SS, et al : Bilateral modified nasoseptal "rescue" flaps in the endoscopic endonasal transsphenoidal approach. Laryngoscope 2013, 123 : 2605-2609,   20. Kim BY, Son HL, Kang SG, Kim SW, Hong YK, Jeun SS, et al : Postoperative nasal symptoms associated with an endoscopic endonasal transsphenoidal approach. Eur Arch Otorhinolaryngol 2013, 270 : 1355-1359,   21. Kitano M, Taneda M : Extended transsphenoidal approach with submucosal posterior ethmoidectomy for parasellar tumors. Technical note. J Neurosurg 2001, 94 : 999-1004,   22. Kobayashi S, Hara H, Okudera H, Takemae T, Sugita K : Usefulness of ceramic implants in neurosurgery. Neurosurgery 1987, 21 : 751-755,   23. Kumar A, Maartens NF, Kaye AH : Reconstruction of the sellar floor using Bioglue following transsphenoidal procedures. J Clin Neurosci 2003, 10 : 92-95,   24. Liu JK, Schmidt RF, Choudhry OJ, Shukla PA, Eloy JA : Surgical nuances for nasoseptal flap reconstruction of cranial base defects with high-flow cerebrospinal fluid leaks after endoscopic skull base surgery. Neurosurg Focus 2012, 32 : E7,  25. Matsumoto K, Kohmura E, Tsuruzono K, Mori K, Kawano K, Tsujimura T : Silicone plate-induced granuloma presenting pituitary apoplexy-like symptoms: case report. Surg Neurol 1995, 43 : 166-169,   26. McCoul ED, Anand VK, Singh A, Nyquist GG, Schaberg MR, Schwartz TH : Long-term effectiveness of a reconstructive protocol using the nasoseptal flap after endoscopic skull base surgery. World Neurosurg 2014, 81 : 136-143,   27. Mehta GU, Oldfield EH : Prevention of intraoperative cerebrospinal fluid leaks by lumbar cerebrospinal fluid drainage during surgery for pituitary macroadenomas. J Neurosurg 2012, 116 : 1299-1303,   28. Mortini P, Losa M, Barzaghi R, Boari N, Giovanelli M : Results of transsphenoidal surgery in a large series of patients with pituitary adenoma. Neurosurgery 2005, 56 : 1222-1233, discussion 1233   29. Nyquist GG, Anand VK, Singh A, Schwartz TH : Janus flap : bilateral nasoseptal flaps for anterior skull base reconstruction. Otolaryngol Head Neck Surg 2010, 142 : 327-331,   30. Patel MR, Taylor RJ, Hackman TG, Germanwala AV, Sasaki-Adams D, Ewend MG, et al : Beyond the nasoseptal flap : outcomes and pearls with secondary flaps in endoscopic endonasal skull base reconstruction. Laryngoscope 2014, 124 : 846-852,   31. Rawal RB, Kimple AJ, Dugar DR, Zanation AM : Minimizing morbidity in endoscopic pituitary surgery : outcomes of the novel nasoseptal rescue flap technique. Otolaryngol Head Neck Surg 2012, 147 : 434-437,   32. Rivera-Serrano CM, Snyderman CH, Gardner P, Prevedello D, Wheless S, Kassam AB, et al : Nasoseptal "rescue" flap : a novel modification of the nasoseptal flap technique for pituitary surgery. Laryngoscope 2011, 121 : 990-993,   33. Seda L, Camara RB, Cukiert A, Burattini JA, Mariani PP : Sellar floor reconstruction after transsphenoidal surgery using fibrin glue without grafting or implants : technical note. Surg Neurol 2006, 66 : 46-49, discussion 49   34. Seiler RW, Mariani L : Sellar reconstruction with resorbable vicryl patches, gelatin foam, and fibrin glue in transsphenoidal surgery : a 10-year experience with 376 patients. J Neurosurg 2000, 93 : 762-765,   35. Shin JH, Kang SG, Kim SW, Hong YK, Jeun SS, Kim EH, et al : Bilateral nasoseptal flaps for endoscopic endonasal transsphenoidal approach. J Craniofac Surg 2013, 24 : 1569-1572,   36. Tomio R, Toda M, Tomita T, Yazawa M, Kono M, Ogawa K, et al : Primary dural closure and anterior cranial base reconstruction using pericranial and nasoseptal multi-layered flaps in endoscopic-assisted skull base surgery. Acta Neurochir 2014, 156( Wien):1911-1915,   37. Yano S, Tsuiki H, Kudo M, Kai Y, Morioka M, Takeshima H, et al : Sellar repair with resorbable polyglactin acid sheet and fibrin glue in endoscopic endonasal transsphenoidal surgery. Surg Neurol 2007, 67 : 59-64, discussion 64  
Fig. 1
A : The first incision was made anteriorly toward the level of one-half to one-third the height of the middle turbinate over the vomer to preserve the nasoseptal pedicle. Then, a curvilinear incision (along the white arrows) was made from the inferior border of the sphenoidal sinus ostium following the sagittal plane of the septum slightly downward. B : By using Cottle and hockey stick elevators, a mucoperiosteal flap was made from the right side of the bony nasal septum and displaced downward into the nasopharynx.

Fig. 2
Modified grading system for cerebrospinal fluid (CSF) leak after endoscopic transsphenoidal surgery.

Fig. 3
Schematic drawing of a lateral view of the sellar floor in grade 3 sellar floor repair. (a) Inlay and (b) outlay dural substitutes with (c) septal bone repositioned, and (d) a pedicled nasoseptal flap is applied at the sellar floor for grade 3 CSF leak repair.

Fig. 4
Endoscopic images of sellar floor repair in grade 3 CSF leak. In cases of large CSF leaks (grade 3), sellar floor reconstruction was performed in a multilayered fashion with (A) oxidative cellulose packing (Surgicel®, Ethicon; Johnson & Johnson), (B) inlay dural substitutes (Duraform®, Codman; Johnson & Johnson), (C) outlay dural substitutes, (D) septal bone, and (E) a pedicled nasoseptal flap. (F) A tissue sealant (DuraSeal®, Covidien) was applied at last.
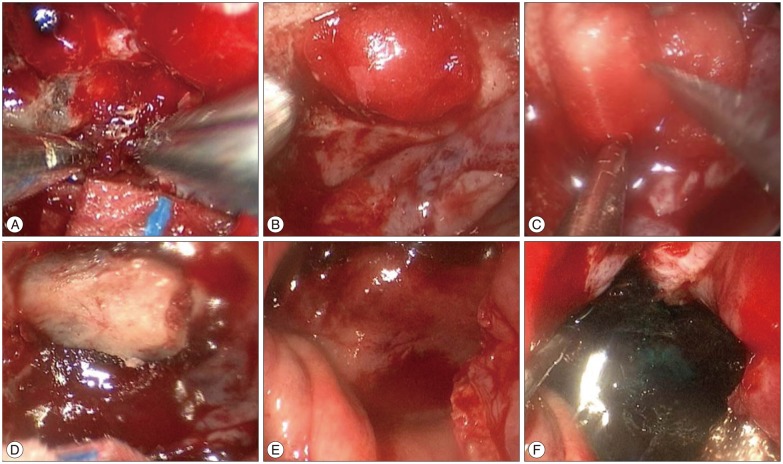
Table 1
Repair protocol for cerebrospinal fluid leak after endoscopic transsphenoidal surgery
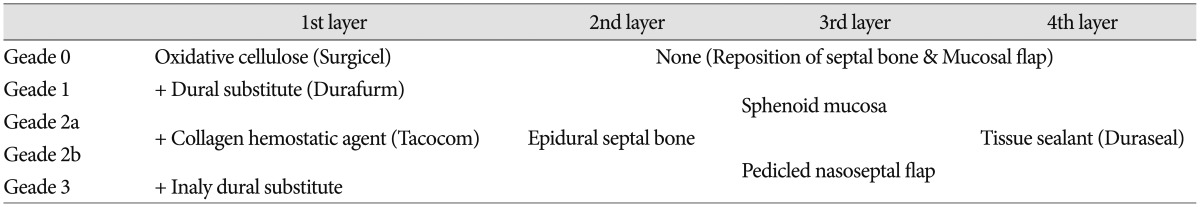
Table 2
Pathologic diagnoses of 188 patients undergoing endoscopic transsphenoidal surgery

Table 3
Intraoperative cerebrospinal fluid leak rates
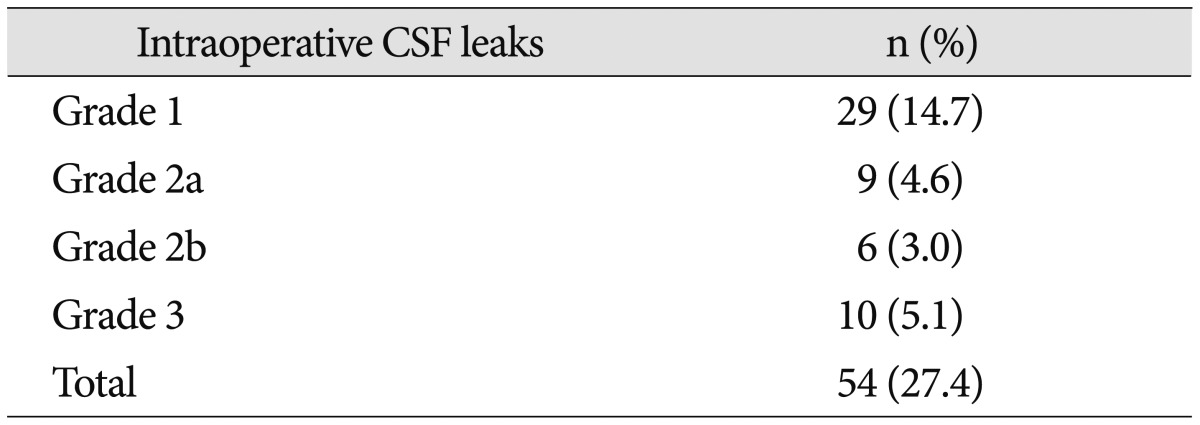
Table 4
Modified grading system and repair protocol for cerebrospinal fluid leak during endoscopic transsphenoidal surgery

Table 5
Other common complications

|
|
























