INTRODUCTION
Traumatic aneurysms arise primarily from the anterior circulation and less frequently from the posterior circulation at a reported incidence of approximately 10%6). Correspondingly, isolated traumatic pseudoaneurysms of the basilar artery are ex-tremely rare because of the secure location of this artery1,6), but are associated with a high mortality, presumably because of pseudoaneurysms growing faster and showing higher rebleeding than true aneurysms8). Therefore, the majority of traumatic basilar artery injuries have been diagnosed in forensic studies. Indeed, to our knowledge, traumatic basilar artery pseudoaneurysm has been reported in only seven clinical cases1,2,3,5,6,8,9). We report here an extremely rare case of traumatic pseudoaneurysm arising from the basilar artery. The traumatic pseudoaneurysm presented with acute pseudoaneurysm formation and rebleeding within the first day after trauma, and was managed with endovascular coil embolization.
CASE REPORT
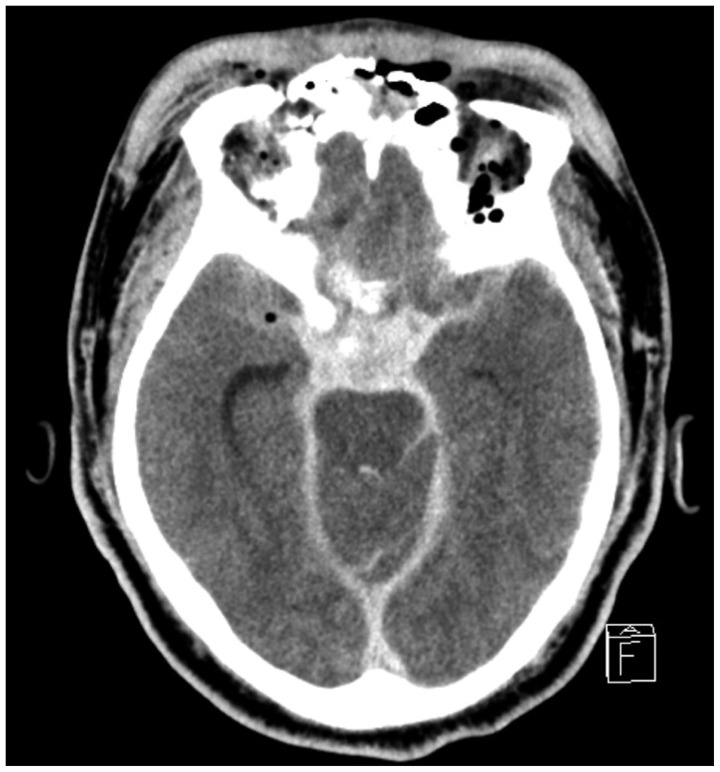
A 51-year-old man was presented to the emergency room after ground-level fall in a state of inebriation. The patient had craniofacial trauma with multiple abrasions, ecchymosis and heavy nose bleeding. On arrival, he was somnolent but was able to obey simple orders (Glasgow Coma Scale : 12). The initial vital signs were stable (blood pressure : 140/100 mm Hg, pulse rate : 80/min). Brain computed tomography (CT) showed thick subarachnoid hemorrhage (SAH) on the basal cistern with clival fracture and traumatic intracranial hemorrhages. Diffuse SAH was predominant in the basal cistern, ambient cistern, left sylvian fissure, prepontine cistern, both cerebellopontine cistern and premedullary cistern (Fig. 1). CT angiography revealed contrast extravasation on the distal basilar artery (Fig. 2). Based on this finding, we decided to conduct conventional angiography for confirming the aneurysm and performing subsequent endovascular management. However, during the preparation of the angiography, the patient fell rapidly into a coma and showed bilateral pupil dilatation (Glasgow Coma Scale : 3). Because of hemodynamic and respiratory instability (blood pressure : 60/40 mm Hg, pulse rate : 120/min), we made the decision to perform conventional angiography after resuscitation. Repeated brain CT revealed the SAH had increased in size (Fig. 3).
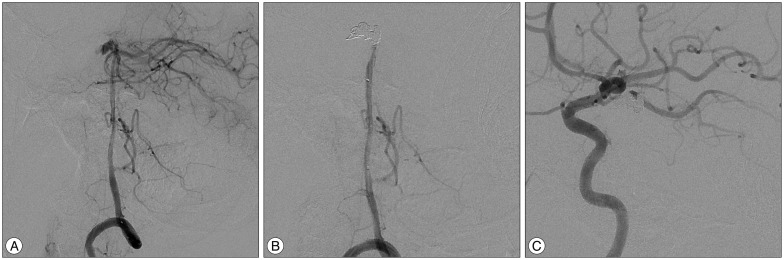
The conventional cerebral angiography confirmed that a pseudoaneurysm arising from the top of the basilar artery corresponded with the contrast extravasation. The size of the aneurysm was 8.5×7.4×3.9 mm. Transarterial coil embolization of the pseudoaneurysm sac and the rupture point of the distal basilar artery was achieved using a double-microcatheter technique (Fig. 4). Following the embolization, bilateral decompressive craniectomy with duraplasty was performed. Although the patient was in intensive medical care, his consciousness did not improve, and he died on the 7th hospital day because of deterioration of his initially poor clinical condition.
DISCUSSION
Traumatic pseudoaneurysms may occur following penetrating or blunt head trauma. For penetrating injury, the mechanism of traumatic aneurysms is direct injury from the bone fragments of skull fractures; in blunt injury, the mechanism is overstretching, torsion, or compression against the dura or bony prominences2,5,8). Traumatic aneurysms of the basilar artery are almost associated with basal skull fractures6), and the arterial wall can be lacerated by a fractured clivus or tentorium secondary to rapid deceleration3,7,9). Traumatic intracranial aneurysms usually become symptomatic after a symptom-free interval following the traumatic episode. In many cases, clinical symptoms or neurologic deterioration of traumatic aneurysms may present within several weeks after the traumatic events2,3,5). Although cerebral angiography cannot reveal a pseudoaneurysm within 1 or 2 days after trauma, a follow-up angiography obtained several weeks later may identify an aneurysm5).
Unlike previously reported cases, the present one showed acute formation of a pseudoaneurysm and deterioration within several hours after trauma due to rebleeding. The authors presumed that overstretching of the perforating artery formed the pseudoaneurysm and that the acute bleeding was arrested temporarily by the adjacent thick hemorrhage. The unexpected rebleeding might have led to serious deterioration because of the increased blood pressure or clot lysis. Because the time interval seem to be short for clot lysis, sudden increased blood pressure was more reliable cause of the rebleeding.
Because of the high mortality associated with traumatic pseudoaneurysms, early diagnosis and prompt treatment are highly important. The several reported treatment options include surgical repair and endovascular embolization4,6). An examination of the recent literature suggests that endovascular treatment has become preferable to surgical repair, and the preference for this treatment option is likely due to traumatic pseudoaneurysms having friable walls and poorly defined neck2,5,6,7,8,9). In our case, endovascular coil embolization was used for the management of the pseudoaneurysm in consideration of the patient's poor clinical condition and the deep location of the pseudoaneurysm. Although occlusion of the parent artery was considered, coil embolization was performed because of the risk of a fatal condition secondary to occlusion of the basilar artery.
The long-term prognosis is heavily influenced by the extent of other primary and secondary brain injuries. Thus, prompt treatment could prevent massive hemorrhage and secondary brain injury, such as brain swelling. Endovascular embolization can be an effective method for the management of pseudoaneurysms, especially posterior circulation aneurysm with poor clinical grade. Furthermore, brain CT angiography should be performed in all patients with traumatic SAH for the identification of possible vascular injury, especially thick SAH around brain stem or SAH with basal skull fractures.
CONCLUSION
This report describes a rare case of traumatic basilar pseudoaneurysm caused by severe SAH within 1 day after trauma. Early detection and prompt management could prevent catastrophic rupture of a traumatic pseudoaneurysm. Therefore, brain CT angiography and endovascular management should be considered for identifying vascular injury in severe traumatic SAH with a basal skull fracture.